Intersphincteric Resection for Patients With Low-Lying Rectal Cancer: Oncological and Functional Outcomes
Article information
Abstract
The aim of this review is to evaluate the outcomes after an intersphincteric resection (ISR) for patients with low-lying rectal cancer. Reports published in the literature regarding surgical, oncological, and functional outcomes of an ISR were reviewed. The morbidity after an ISR was 7.7%–32%, and anastomotic leakage was the most common adverse event. Local recurrence rates ranged from 0% to 12%, 5-year overall survival rates ranged from 62% to 92%, and rates of major incontinence ranged from 0% to 25.8% after an ISR. An ISR is a safe procedure for sphincter-saving rectal surgery in patients with very low rectal cancer; it does not compromise the oncological outcomes of the resection and is a valuable alternative to an abdominoperineal resection. While the functional outcomes after an ISR were found to be acceptable, the long-term functional outcome and quality of life still require careful investigation. ISRs have been performed with surgical and oncologic safety on patients with low-lying rectal cancer. However, patients must be selected very carefully for an ISR, considering the associated functional derangement and the limited extent of the resection.
INTRODUCTION
Rectal cancer treatments have dramatically advanced in recent decades. Despite the evolution of adjuvant chemoradiation therapy, radical surgical treatment remains the most fundamental approach to treating patients with rectal cancer. The surgical treatment of such patients includes complete tumor removal to diminish the risk of recurrence and to preserve the quality of life. As one of the great advances in the field of surgical treatment for patients with low-lying rectal cancer, the sphincter-saving resection without a permanent stoma has been performed extensively in recent years instead of an abdominoperineal resection (APR). This is due to a better understanding of tumor spread and lymphatic drainage patterns and to advances in surgical technologies, such as improved stapling devices and double stapling techniques [1-3].
The discovery of the importance of the total mesorectal excision in achieving local tumor control and higher survival rates [4] has reduced the number of patients requiring permanent colostomies. In addition, a better understanding of the optimal safe distal resection margin has allowed increased incidences of sphincter-sparing resections. Reduction of the distal margin from 5 to 2 cm, or even 1 cm, has increased the frequency of sphincter-saving resections without compromising oncologic results [5]. In most instances a distal margin of 1–2 cm is currently considered sufficient for ultra-low rectal cancer [5-8].
In recent years, additional efforts have been made to improve the rate of sphincter preservation. The most extreme form of rectal resection is an intersphincteric resection (ISR) with coloanal anastomosis (CAA) [6-18]. The ISR was introduced in the 1990s to avoid permanent colostomy and has been increasingly performed as the ultimate surgical treatment for patients with a rectal cancer that is located at or near the dentate line. For very low-lying tumors, safe distal margins can only be achieved by using a partial or a total resection of the internal sphincter or by using an APR. Because ISR preserves the external sphincter and anal canal, there are concerns regarding an increase in the risk of local recurrence due to insufficient distal or circumferential margins after resection. Indeed, a partial or a total resection of the internal anal sphincter can interfere with fecal continence [6, 9-13, 15]. However, several investigators have reported satisfactory long-term oncologic and functional outcomes [14, 15, 17-19].
Although the ISR has been associated with certain controversial functional results, its benefit of “no stoma” has been widely accepted. A majority of patients prefer sphincter preservation rather than permanent colostomy. However, the decision to proceed with a sphincter-preserving procedure rather than an APR for patients with low-lying rectal cancer must be based on the careful consideration of many factors.
MORBIDITY AND MORTALITY
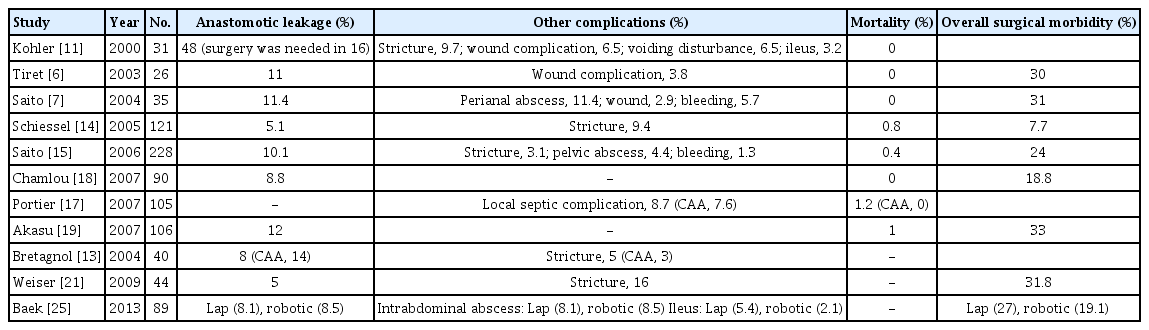
Reported mortality and morbidity rates after an ISR range from 0% to 5% and from 7.7% to 32%, respectively [8, 14-16, 18], which are not significantly different from those reported after a low anterior resection (LAR) or APR [16, 19] (Table 1). The most frequent early complication was anastomotic leakage, although patients with anastomotic leakage rarely seemed to require any additional surgery to resolve this complication. In certain studies, anastomotic leakage rates up to 16% have been mentioned [13, 14, 17-21].
Many research reports have compared surgical complications after an ISR with those that occur after a LAR. Weiser et al. [21] reported on the morbidity following LAR/stapled CAA and LAR/ISR/hand-sewn CAA, in addition to APR. Regarding their study, anastomotic leakage was not significantly different between the ISR and the LAR. Surgical complications were observed in 31.8% of patients after an ISR and in 9.7% of patients after a LAR. Portier et al. [17] reported a local septic complication rate after an ultralow CAA comparable to that of a partial ISR and CAA without an ISR. However, some early studies have shown high complication rates after an ISR. Köhler et al. [11] reported an anastomotic leakage rate that was higher than those that were usually reported. In their study, 48% of the patients experienced anastomotic leakage, and 16% of the patients required surgery. They suggested that the high anastomotic leakage rate in their study might be attributed to the exact postoperative controls that were associated with the detailed documentation. They defined suture insufficiencies as impairments in the healing of the anastomosis that were detected radiologically and/or rectoscopically. They suggested that small insufficiencies in the anastomotic plane were often not verifiable radiologically due to the location of the anastomosis and that rectoscopic examination enabled the recognition of smaller leakages. This may explain, they claim, the observation that the total rate of anastomotic leaks in their study was 48%. With the exception of Kölher`s study, the anastomotic leakage rate in the literature is reportedly comparable to that after CAA without an ISR.
Other than anastomotic leakage, anastomotic stricture, which may be the end result of anastomotic leakage or ischemia, was a frequently reported complication. Anastomotic strictures have also been reported after stapled anastomosis for sphincter-saving surgery. A review of the literature reveals that the incidence of rectal anastomotic narrowing varies from 0% to 30% [6, 22, 23]. Comparison of the anastomotic stricture rates was difficult because the definition of stricture varies, and few authors provided their precise definition of stenosis. Nevertheless, anastomotic stricture rates after an ISR have been reported to range from 3.1% to 16%, which are comparable to those after stapled anastomosis [15-21]. The frequencies of other surgical morbidities after an ISR, such as wound complications, bleeding, and ileus, have been reported to range from 7% to 31% [15-21].
The use of laparoscopic and robotic approaches has increased over time. Robot approaches, especially, have been used more frequently for treating patients with low-lying rectal cancer due to their technical benefits. Surgical complications do not differ among approaches. Park et al. [24] compared surgical and oncological outcomes between laparoscopic and open ISR and found that the overall complication rates for the two approaches were similar (laparoscopic 5.4% vs. open 3.8%, P = 0.428). Baek et al. [25] directly compared robotic and laparoscopic ISR and observed that complication rates did not differ between the 2 approaches. Similar anastomotic leakage rates have been reported for laparoscopic (8.1%) and robotic approaches (8.5%).
Similar surgical morbidities, regardless of approach, have been reported by many studies, and it has been suggested that an ISR can be performed with surgical safety similar to that for laparoscopic, robotic, and open approaches [26-29]. However, definitive benefits from one specific approach, over the other approaches, have not been elucidated.
ONCOLOGICAL OUTCOMES
Local control is one of the most important oncological objectives in surgery on patients with low-lying rectal cancer. Local recurrence rates ranging from 4% to 13% have been reported following sphincter-saving resections for low-lying rectal cancer [4, 5, 30, 31]. Several specialized studies that investigated an ISR for treating patients with low-lying rectal cancer have reported local recurrence rates that ranged from 0% to 12% [6-8, 11, 12]. Among the studies, the inclusions of patients with and treatments involving either neoadjuvant or adjuvant therapies were significant. In a previous series of ISRs [14], a 5.3% rate of local recurrence was reported among the 113 patients who had undergone an ISR; among whom, 31% of the patients had T3 tumors, 37% of which were stage III lesions that had not received radiotherapy. On the other hand, Rullier et al. [12] reported that one (2%) of 58 patients (88% of whom received preoperative radiotherapy), mostly with T3 tumors, developed local recurrence during a median follow-up period of 40 months. Recent series have included more patients who were treated with preoperative chemoradiotherapy (PCRT) [12, 25, 26], and some studies have compared oncologic outcomes after an ISR between patients who were treated with PCRT and those who were not [27, 32]. Local recurrence was not found to differ according to PCRT. In addition, the local recurrence rate was not influenced by the surgical approach [24-28].
Recurrence-free survival and overall survival after an ISR have also been steadily investigated to evaluate the oncologic safety of an ISR for patients with low-lying rectal cancer. Saito et al. [15, 32] reported data from patients who were treated with an APR and an ISR and who underwent surgery during the same time period. Although there was a concern of an increased local recurrence rate in patients who were treated with an ISR because of the surgical margins being smaller compared to those for an APR, the cumulative 5-year local recurrence rate was 6.7% in their series. Patients who were treated with an APR displayed tumors of the same background compared to patients who received an ISR, and the median 5-year local recurrence rate was 10%. In a more recent study, the authors reported long-term oncologic outcomes after an ISR and an APR. The 5-year overall survival rates were 80% for the ISR and 61.5% for the APR, and the 5-year disease-free survival rates were 69% for the ISR and 73% for the APR. However, one must consider differences of surgical indication between the ISR and the APR.
Weiser et al. [21] compared oncologic outcome in patients with locally advanced, ultra-low rectal cancers who were treated with chemoradiation, followed by either a LAR and stapled CAA, an ISR and hand-sewn CAA, or an APR with permanent colostomy. Although the local recurrence rates did not show statistically significant differences among the three groups (LAR/stapled CAA vs. LAR with ISR vs. APR; 2% vs. 0% vs. 9%, P = 0.16), recurrence-free survival was profoundly lower in the APR group (85% vs. 83% vs. 47%). Rullier et al. [12] studied patients who underwent an ISR for T3 or T4 disease and had received preoperative chemoradiotherapy. He reported an 85% 3-year survival rate and an 85% 3-year disease-free survival rate. Akasu et al. [19] studied 106 patients who underwent an ISR without radiotherapy. Thirty-eight patients had stage III disease in their study, and without any kind of radiotherapy, the 3-year overall survival rate was 95% after a median follow-up of 41 months. During the follow-up period, 4% of the patients with stage I, 5% with stage II, and 18% with stage III disease developed distant metastases.
A recent series that compared long-term oncologic outcomes after an ISR performed by using a minimally invasive approach showed results similar to those that were obtained following an open ISR [24-28]. Determination of the necessary distal resection margin length did not impact the local recurrence rate. Recent studies have also shown that intramural tumor extension beyond the gross mucosal edge is uncommon and generally less than 1 cm [33, 34]. An additional analysis showed no differences in outcomes between patients with distal margins that were either greater than or less than 1 cm in the setting of PCRT [35].
Involvement of the radial margin is the most important predictive factor for local recurrence after rectal cancer resection and is known to influence survival [36-39]. Achieving negative radial margins for carcinomas that are located in the lower third of the rectum remains a challenge because at this level, the mesorectum is either thin or lacking. This is the main contraindication for a sphincter-saving resection in patients with T3 lower rectal tumors. PCRT decreases the tumor volume, induces downstaging, and facilitates surgical resection. In addition, PCRT transforms the tumor into an ulcerative scar, which may decrease intraoperative tumor seeding.
Hohenberger et al. [16] reported a 25.1% local recurrence rate following an ISR and found that 14.2% of the patients who were treated with PCRT developed local recurrences. They suggested that PCRT might increase local control for patients who have indications for an ISR; however, the effects of PCRT still remain controversial. The local recurrence rate, at a mean follow-up of 40 months, was 2% in the Rullier series of 92 patients with mostly T3 tumors (72 of the 98 patients) [8], and 81 of those 92 patients (88%) had received PCRT. Bonadeo et al. [40] observed a higher recurrence rate for very low T3 rectal tumors in the absence of radiotherapy, and Saito et al. [7] reported similar results for local control, with acceptable anal functions, in a series of 35 patients (median follow-up: 23 months). Saito et al. [7] also observed comparable results between patients with T3–T4 disease who underwent PCRT and those with T2 disease who did not undergo PCRT.
Some researchers [11, 14, 19] have reported good local control and survival rates without PCRT; however, patients with locally advanced, low-lying rectal cancers who received PCRT exhibited improved oncological outcomes. The wide use of PCRT has facilitated the application of an ISR to patients with low-lying rectal cancers. Based on the results of the studies described above, besides the certain controversial issues that are related to PCRT, such as its role in sphincter preservation, PCRT plays a role in the facilitation and safe application of ISR for patients with low-lying rectal cancer. The oncological outcomes after an ISR are summarized in Table 2.
FUNCTIONAL OUTCOMES
For patients who undergo surgical treatment for rectal cancer, their postoperative quality of life remains a major issue that is largely defined by an acceptable level of continence. For low anastomoses, in general, a greater incidence of urgent defecation, incontinence for all qualities of stool, and evacuation disorders, together with increased stool frequencies, have been observed [41, 42]. Unquestionably, the functional results are more problematic if the location of the anastomosis is low [41-43]. Therefore, impaired continence has been asserted to be an inevitable consequence of an intersphincteric rectal resection [9, 10]. The impaired control of defecation after a LAR is undoubtedly multifactorial. Direct trauma to the sphincter muscles and an interruption, at least temporarily, of reflex mechanisms can occur, and the physiological properties of the neorectum greatly differ from normal [43, 44].
Concerns exist about the long-term functional outcomes after an ISR, even though an ISR is technically feasible and oncologically safe, because the loss of the rectum and the internal anal sphincter may induce anal dysfunction, such as changes in stool frequency, urgency, fragmentation, soiling, and fecal incontinence. The high percentage of patients with anterior resection syndrome after a stapled low colorectal or high coloanal anastomoses, [42, 44, 45] despite entire preservation of the anal sphincter, suggests that factors other than the anal sphincter are involved in incomplete fecal function after a rectal resection. The loss of rectal reservoir function seems to be a crucial factor [43] that explains why the level of anastomosis [44, 45] has been reported to influence the quality of continence after a rectal resection. In addition, PCRT usually includes the anal sphincter in patients with low-lying rectal cancers, and the irradiation has a deleterious impact on anorectal function [18, 46, 47].
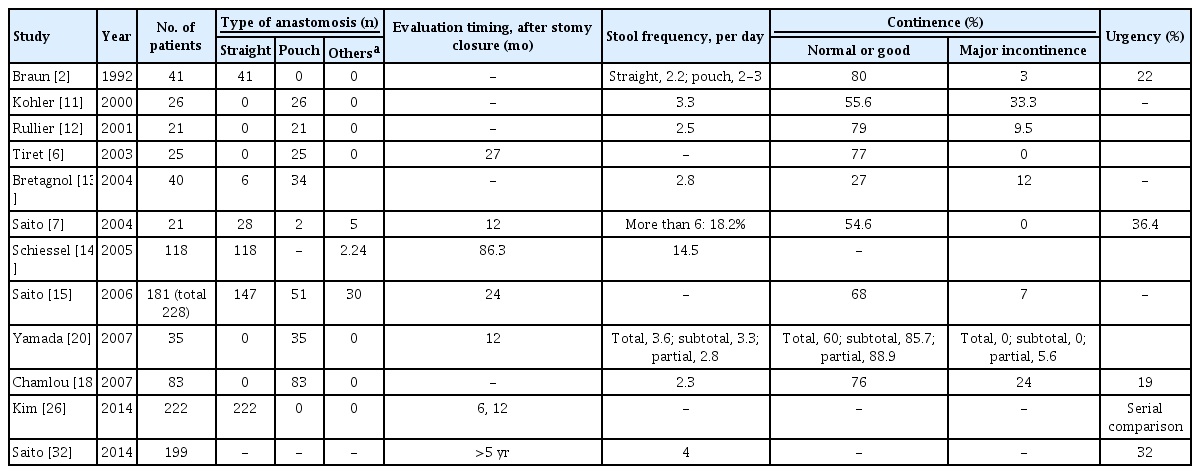
Although the postoperative fecal dysfunctions that are caused by partial or complete excision of the internal anal sphincters have been a concern in relation to an ISR, some studies have demonstrated relatively satisfactory defecatory functions after an ISR [6, 12-14, 20]. Various researchers have reported diverse continence levels after an ISR, which included normal continence (29% to 86.3%), major incontinence (0% to 25.8%), and need-for-colostomy (0% to 0.8%) [6, 12, 14, 15, 18, 20] (Table 3).
Some authors have tried to explain the cause of fecal incontinence after an ISR by means of physiologic studies. Fecal incontinence after an ISR is primarily caused by anal-sphincter insufficiency. Physiologic studies have shown that removal of the internal anal sphincter is associated with a significant decrease in resting pressure [7, 9]. The maximum resting anal canal pressure is maintained by the internal anal sphincter. This pressure, as expected, reportedly fell after an ISR, although a gradual rise was subsequently observed.
Neorectal insufficiency may cause fecal incontinence, as demonstrated by randomized studies that compared straight and J-pouch coloanal anastomoses [12, 13, 48]. Based on experience with the ileal J-pouch, suggested suggestion was made that the functional results may improve after very low rectal resections because of an increased neorectal volume. Not only does the pouch increase the maximum tolerable volume, but it also potentially acts as a motility brake [48]. Cluster defecation that is associated with tenesmus, urgency, and incontinence is not uncommon in straight CAA. The colonic pouch could convert the functional deficiencies that are associated with the loss of rectal capacity and reduce compliances that result from straight CAA.
Due to good functional results, the colonic J-pouch anal anastomosis has gained general acceptance and is becoming the operation of choice for patients with carcinomas in the lower third of the rectum. Several authors have advised performing a pouch anastomosis to improve functional outcomes [44, 48]. A meta-analysis has also revealed minimal differences in functional outcomes between the pouch and the straight CAA at one year, and anastomotic stricture seems more likely to occur after a pouch-anal anastomosis [49]. Currently, the colonic pouch has short-term functional advantages that are widely accepted, but few long-term advantages.
Although some authors have questioned the advantages of an ISR for treating patients with low-lying rectal cancers in terms of quality of life [50], compared to CAA, a permanent colostomy must be considered as a serious handicap. Indeed, with the addition of a colonic pouch, the results of CAA have significantly improved over the past decade, even though it was found primarily to confer only a short-term benefit.
CONCLUSIONS
An ISR is a safe procedure for sphincter-saving rectal surgery in patients with very low rectal cancer and is a valuable alternative to an APR. Compared to an APR, recurrence and survival are not compromised, and acceptable oncological and functional results have been obtained using ISR procedures. Therefore, ISR can be recommended for patients who are APR candidates; however, information on the potential for functionally adverse effects after an ISR should be preoperatively provided to the patients.
Laparoscopic and robotic ISRs have also been reported to be safe and efficient procedures for select patients and have been associated with reduced postoperative pain, decreased disability, shorter hospitalization, and better cosmesis. Because anastomosis was performed transanally in most cases, a laparoscopic procedure may be more efficiently used for an ISR.
Recently, PCRT has become widely applied for the treatment of patients with low rectal cancer. PCRT reportedly induces tumor downstaging and affords the potential for preserving the sphincter in patients with very low rectal cancer. Neoadjuvant chemoradiation allows an ISR to be applied to a greater number of patients without compromising the oncologic outcome. In fact, by using a multimodal approach, an ISR was found to be practical, even in patients with advanced cancer of the lower rectum.
Anorectal function is acceptable in the majority of patients, but compared with conventional CAA, this technique exposes the patients to risk of worse continence, but with only a slightly improved quality of life. In addition, in patients with very low rectal cancers, preoperative radiotherapy usually includes the anal sphincter, and the irradiation deleteriously influences anorectal function. The influences of adjuvant treatments, in particular preoperative radiochemotherapy, on the functional outcomes of an ISR remain to be established. Thus, ISR should lead to a decrease in the number of APRs that are performed on patients with very low rectal tumors, although evaluations of the long-term functional outcome and patients’ qualities of life are still required.
Notes
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.
Acknowledgements
Financial support for this project was provided by the Korea Research Foundation (Grant/Award Numbers: 2016R1E1A1A02919844 and 2017R1A2B1009062), Ministry of Science, ICT, and Future Planning, Republic of Korea.