- Search
|
|
Abstract
Purpose
Mucinous adenocarcinomas account for about 10% of all colorectal cancers. This study aimed to investigate the prognostic impact of mucinous histologic subtype on oncologic outcomes in patients with colorectal cancer.
Methods
This retrospective study was performed at two large tertiary university hospitals. We analyzed the characteristics, prognostic factors, and survival of patients with colorectal cancer who were treated and followed up between 2000 and 2013.
Results
Totally, 144 of 1,268 patients with a colorectal adenocarcinoma (11.4%) had mucinous histologic subtype. Statistically significant results found in this research are as follows: Mucinous histologic subtype tended to present in younger patients and to have larger tumor size, higher histologic grade, higher node stage, larger number of positive nodes, and higher rate of perineural invasion compared to nonmucinous histologic subtype. On the univariate analysis, mucinous subtype was a prognostic factor for disease-free and overall survival. On the multivariate analysis, primary tumor location, node stage and lymphatic-vascular invasion were independent prognostic factors for the local control rate. Rectal tumor location, higher disease stage, tumor grade II, and presence of lymphatic-vascular invasion had negative influences on disease-free survival, as did rectal tumor location, higher disease stage and presence of lymphatic-vascular invasion on overall survival.
Colorectal cancer is the third most common cancer in the world [1]. In Iran, colorectal cancer is the fifth common cancer among men and the third among women [2]. A mucinous colorectal carcinoma (MCC) is histologically defined as a tumor with more than 50% extracellular mucin. This pathologic subtype comprises 10%–15% of all colorectal cancers [3,4]. Although the prognostic significances of several characteristics, including the TNM stage, tumor grade, preoperative carcinoembryonic antigen (CEA) level, lymphovascular invasion, and surgical margin status, have been clearly established in patients with colorectal cancer, the effect of mucinous histology on tumor local control (LC) and overall survival (OS) is still under debate [5,6,7]. In most series, a predilection exists for the MCC to occur in the right colon; however, some reports indicate the sigmoid colon and the rectum as being common locations for a MCC, as well [8,9]. Furthermore, an association exists between the mucinous subtype and adverse pathological features in patients with colorectal cancer. MCCs tend to have larger tumor size, higher histologic grade, higher primary tumor and node stage, higher number of positive nodes, higher rate of perineural invasion, and more frequent high-frequency microsatellite instability compared to nonmucinous colorectal carcinomas (NMCCs) [4,10]. Currently, mucinous histology does not influence treatment decision-making for this cancer [11]. However, evidence has suggested that a MCC is a biologically distinct disease requiring special clinical consideration and treatment strategy [12,13,14]. This study aims to investigate the clinicopathological features of MCCs and to identify the relationship between this histology and patients' oncologic outcomes.
This retrospective study was performed at two large tertiary academic hospitals. We analyzed the characteristics, prognostic factors, and survival of patients with colorectal cancer who were treated and followed up between January 2000 and December 2013. This study was approved by the local university's ethics committee in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki. The median follow-up was 62 months for the surviving patients. Tumor staging was performed using the seventh edition of the American Joint Committee on Cancer (AJCC) TNM staging system [1]. In this study, mucinous histologic subtype was defined as being composed of more than 50% extracellular mucin. All tumors were graded according to the World Health Organization standard for tumors of the digestive system. Tumor grading was determined using the content and the appearance of glandular structures between histologic subtypes. Preliminary evaluation included comprehensive history and physical examination, colonoscopy, complete blood cell count, liver and renal function studies, CEA level, and chest, abdominal, and pelvic computed tomography scans. Moreover, a standard open or laparoscopic surgery was performed for the colectomy, low anterior resection, or abdominoperineal resection in 1,126 patients (88%).
Chemotherapy consisted of intravenous bolus 5-fluorouracil (425 mg/m2/day) and leucovorin (20 mg/m2/day) on days 1 to 5 every 3 weeks. Monotherapy with oral capecitabine (825 mg/m2) was administered twice daily for 14 days every 3 weeks, and capecitabine (1,000 mg/m2) was administered twice daily for 14 days every 3 weeks plus oxaliplatin (130 mg/m2) intravenously on day 1 ([capecitabine + oxaliplatin (CAPEOX) regimen]) or oxaliplatin (5 mg/m2) on day 1 plus a 2-hour infusion of leucovorin (200 mg/m2) on days 1 and 2, followed by bolus 5-FU (400 mg/m2) and then 5-FU (600 mg/m2) over a 22-hour infusion on days 1 and 2 every 2 weeks ([oxaliplatin + 5-fluorouracil + folinic acid (FOLFOX) regimen]). Additionally, capecitabine monotherapy or bolus 5-FU/leucovorin was used for concurrent chemotherapy in cases that received neoadjuvant or adjuvant chemoradiation.
Clinical and pathologic variables were analyzed using the IBM SPSS Statistics ver. 19.0 (IBM Co., Armonk, NY, USA). Categorical variables of patients' demographics (such as sex and categorized age), tumor characteristics (such as stage, grade, surgical marine status, lymphatic vascular invasion, perineural invasion, and categorized tumor size), and treatment modalities (such as adjuvant radiotherapy) were compared using the chi-square test. On the other hand, the Student t-test was used for continuous variables, such as patients' ages and tumor sizes. Proportions were also compared through Fisher exact test for unordered or ordered categorical variables. Moreover, univariate analyses for LC, disease-free survival (DFS), and OS rates were carried out using the Kaplan-Meier method, and prognostic factors were compared using the log-rank test. Furthermore, multiple-covariate analyses were performed using the stepwise regression hazards regression model. The hazard ratio for death with a 95% confidence interval was calculated for the variable groups. The log-rank test was also employed to compare the treatment results in each variable group. All the statistical tests were 2-sided, and P-values less than 0.05 were considered to be statistically significant.
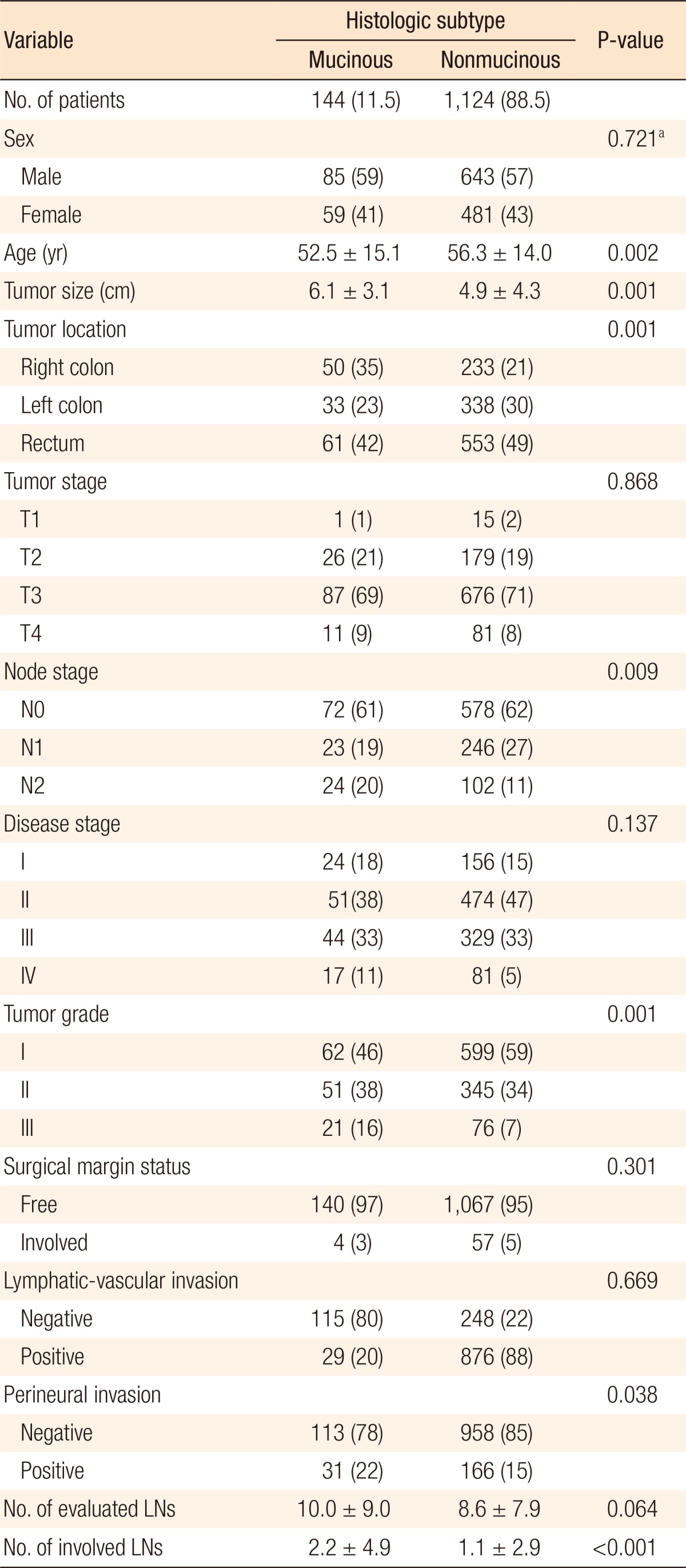
The study subjects included 540 female and 728 male subjects with an age range from 17 to 90 years. The median age at diagnosis was 56 years for all the patients. Among the 1,268 patients with a colorectal adenocarcinoma, 144 (11.4%) had a mucinous histologic subtype. The peak frequency was observed between the sixth and the seventh decades of life in both genders. In the MCC group were 85 male and 59 female subjects with a mean age of 52.5 years (range, 22–84 years). In the NMCC group were 643 male and 481 female subjects with a median age of 56.3 years (range, 17–90 years). The results showed a significant difference between the MCC and the NMCC groups regarding the patients' mean age (52.5 ± 15.1 years vs. 56.3 ± 14.0 years, P = 0.002). However, no significant difference was found between the 2 groups concerning the male/female ratio (1.4 vs. 1.3, P = 0.721).
A comparison of the clinicopathologic characteristics of the 144 patients with a MCC to those of the 1,124 patients with a NMCC is presented in Table 1. Compared to the patients in the NMCC group, those in the MCC showed a predilection for the tumor's location to be in the right colon and the sigmoid colon (P = 0.005). In addition, in the MCC group, the tumors tended to have larger size (P = 0.004), higher histologic grade (P = 0.001), higher node stage (P = 0.009), larger number of positive nodes (P < 0.001), and higher rate of perineural invasion (P = 0.038). However, no statistically significant differences were observed between the MCC and the NMCC groups in terms of surgical margin status, pathologic tumor stage (T-stage), AJCC stage, and presence of lymphatic vascular invasion.
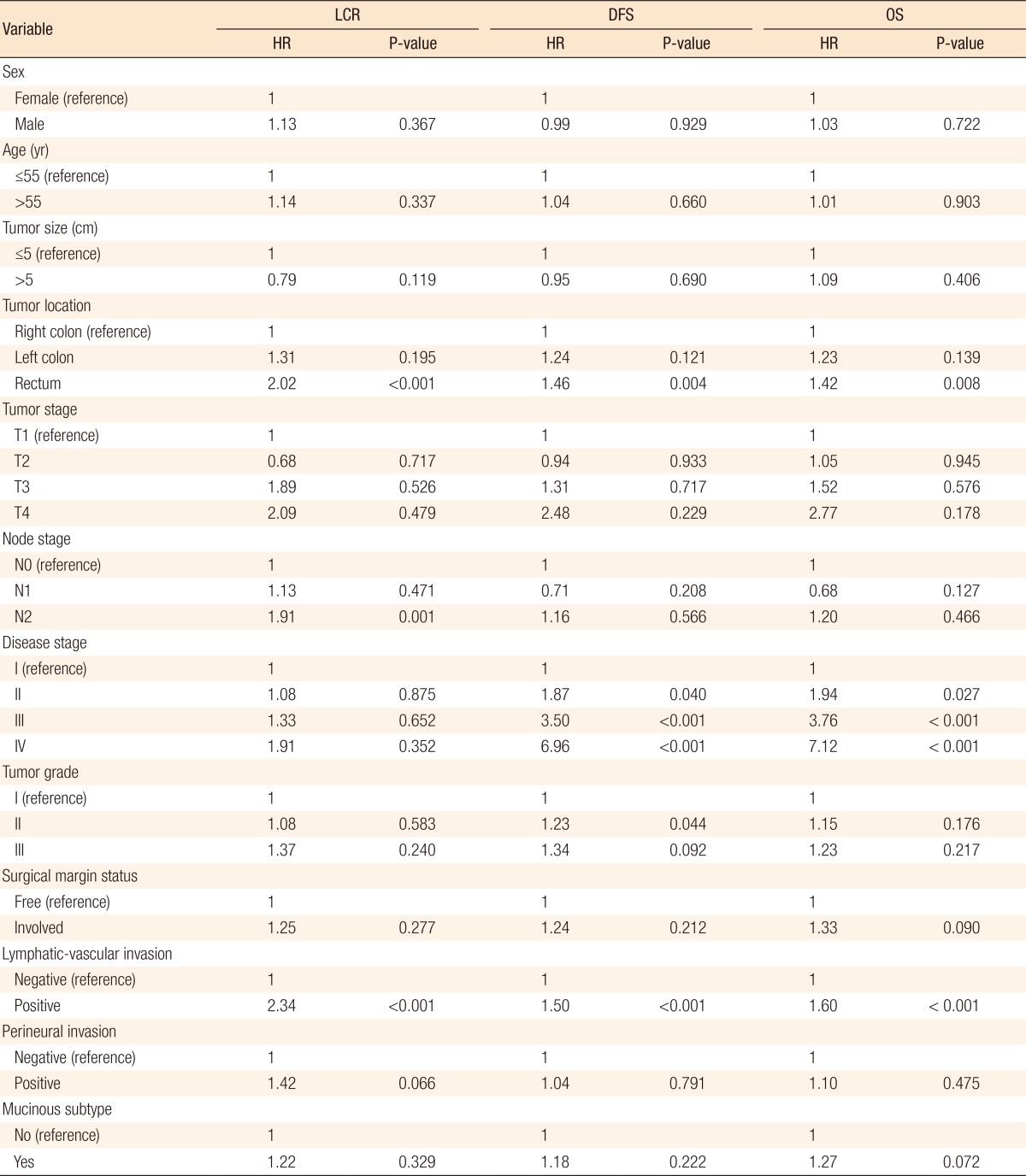
The 5- and the 10-year LC rates for the patients in the MCC group were 78.4% and 76.4%, respectively. On the univariate analysis, the primary tumor location (P = 0.001), lymphatic-vascular invasion (P < 0.001), and perineural invasion (P = 0.047) were found to be prognostic factors for LC. On the multivariate analysis, the primary tumor location, node stage and lymphatic-vascular invasion were found to be independent prognostic factors for LC. Rectal tumor location (P < 0.001), N2 node stage (P = 0.001) and presence of lymphatic-vascular invasion (P < 0.001) had negative impacts on LC.
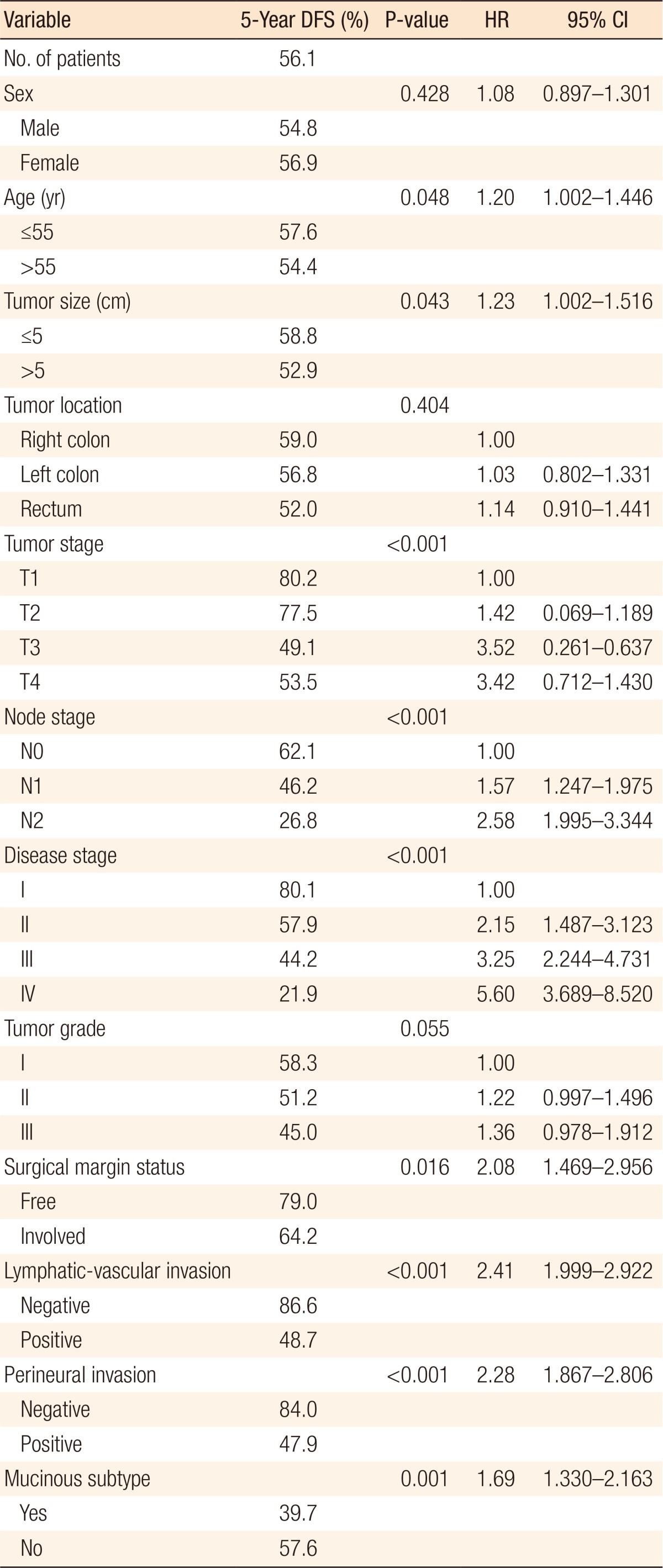
The 5- and the 10-year DFS rates for all the patients with colorectal cancer were 56.1% and 53.0%, respectively. On the univariate analysis, tumor stage (P < 0.001), node stage (P < 0.001), disease stage (P < 0.001), surgical margin status (P = 0.016), lymphatic-vascular invasion (P < 0.001), mucinous subtype (P = 0.001) (Fig. 1), and perineural invasion (P < 0.001) were found to be prognostic factors for DFS (Table 2). On the multivariate analysis, on the other hand, rectal tumor location (P = 0.004), higher disease stage (P < 0.001), tumor grade II (P = 0.044), and presence of lymphatic-vascular invasion (P < 0.001) had negative influences on DFS.
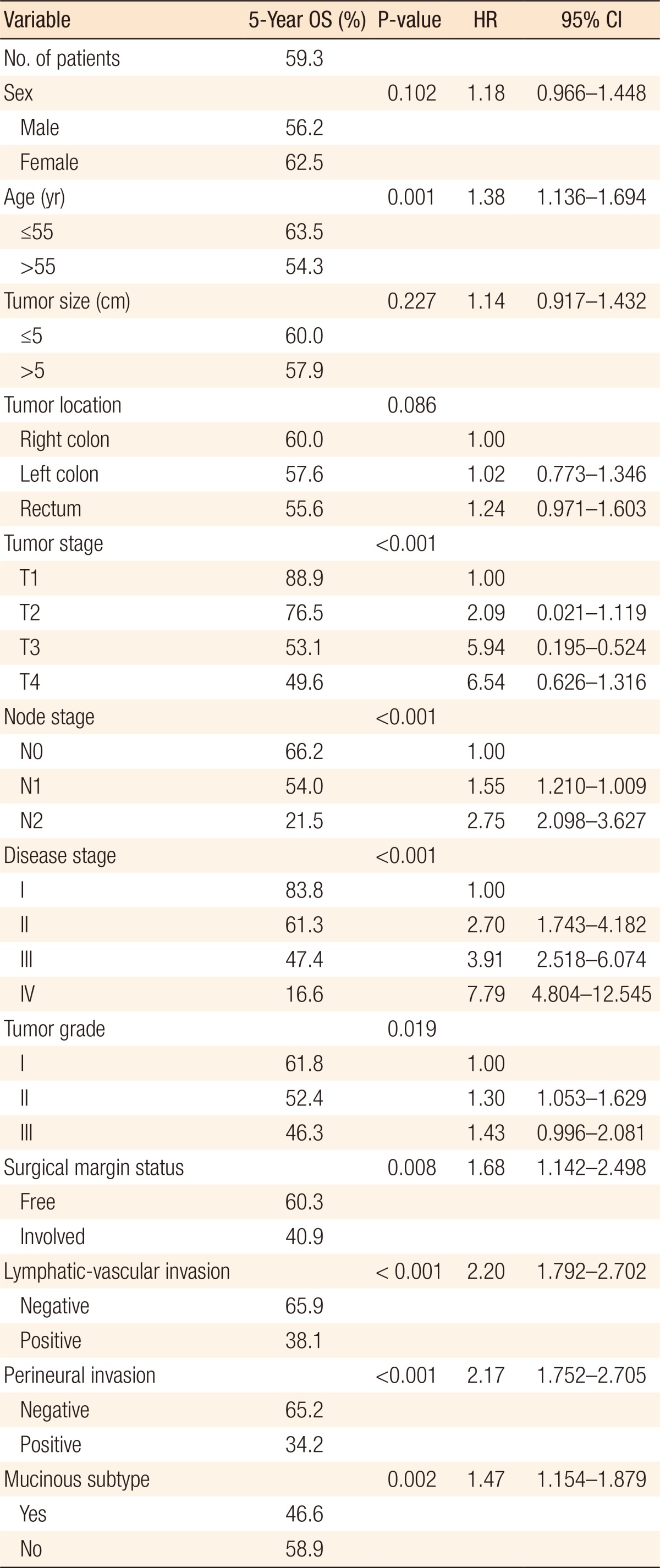
The 5- and 10-year OS rates for all the patients with colorectal cancer were 59.2% and 54.5%, respectively. On the univariate analysis, age (P = 0.001), tumor stage (P < 0.001), node stage (P < 0.001), disease stage (P < 0.001), lymphatic-vascular invasion (P < 0.001), perineural invasion (P < 0.001), tumor grade (P = 0.019), mucinous subtype (P = 0.002) (Fig. 2), and surgical margin status (P = 0.008) were found to be prognostic factors for OS (Table 3). On the multivariate analysis, primary tumor location, disease stage and lymphatic-vascular invasion were also found to be independent prognostic factors. Indeed, rectal tumor location (P = 0.008), higher disease stage (P = 0.001), and the presence of lymphatic-vascular invasion (P < 0.001) negatively influenced the OS (Table 4).
This study aimed to analyze the data on 1,286 patients with a colorectal adenocarcinoma at 2 large tertiary centers in Iran. The incidence rate of mucin histology was 11.4%, which is higher the incidence rates in the majority of reports from Asia (generally between 3% and 9%) [6,15,16,17] and corresponds to the incidence rates reported in Western countries (from 11% to 20%) [18,19,20]. This finding may reflect a biological change in colon cancer, probably caused by a change in dietary habits and lifestyle [21].
In contrast to the predominance of MCC in females reported in several studies [22,23,24], the male-to-female ratio was 1.4 in the present study. This result was similar to that obtained in another Iranian report by Safaee et al. [9]. According to previous studies, a MCC is usually found in populations of younger age and originates from the proximal colon. Moreover, MCCs often present with large size, high nuclear grade, high rate of lymph-node metastasis, and advanced stage [4,13,20,25]. These characteristics were mostly in agreement with the results for our patients. In this study, the most consistent prognostic factors for the patients' LC, DFS, and OS were TNM stage and lymphatic-vascular invasion. Also, based on multiple powerful trials, the College of American Pathologists identified, with a high level of confidence based on ample evidence, the TNM stage and lymphovascular invasion in category I, as prognostic factors [26]. In addition, this study found primary tumor location to be an independent prognostic factor for LC, DFS and OS. Prior studies showed that the difference in oncologic outcomes between patients with a MCC and those with a NMCC is mostly related to tumors with a rectal location. In fact, patients with a MCC tend to have more frequent local recurrence, which supports our present results [25].
When the patients' survival was considered, the presence of a MCC was not an independent prognostic factor in our cohort. Nevertheless, contradictory results have been obtained from the literature regarding the impact of mucinous histology on patients' survival. Similar to our results, Purdie and Piris [19] and Xie et al. [27] did not find the presence of a mucinous adenocarcinoma to be an independent prognostic factor for patients with colorectal cancer. However, some studies have reported a lower survival rate in patients with a MCC [15,22,24]. Surprisingly, Hogan et al. [28] showed an improved survival in patients with a mucinous carcinoma of the colon. These discrepancies may reflect heterogeneity in the population of patients, lack of stratification by stage, exclusion of rectal primary tumors in some studies, and different numbers of patients accrued.
Nitsche et al. [12] and Numata et al. [25] reported the adverse effect of mucin production on LC, which was confirmed in our study. Our findings demonstrated an increased risk of local recurrence in patients with tumors located in the rectum. This finding may be due to the lymphatic drainage of the pelvis being more extensive than that of the colon [29]. Whether patients with a MCC should be managed with a specific treatment strategy different from the strategies used to treat patients with a classical adenocarcinoma is not known. Recent trials have suggested a lower response to neoadjuvant chemoradiation for patients with a mucinous carcinoma [30,31]. Numata et al. [25] concluded that as MCCs are more likely to be locally recurrent, intensified management of LC in patients with a MCC should result in improved OS.
The limitations of this study are important to note. The first limitation is its retrospective nature, which may be intrinsically associated with an imbalance of patients and tumor characteristics. The second limitation is the modest number of patients in the mucinous subtype arm, which may preclude detection of very small differences. Hence, further well-designed, multicentered, prospective trials should evaluate any need for histology-based treatment modulation in patients with colorectal cancer.
ACKNOWLEDGMENTS
The authors would like to thank Ms. A. Keivanshekouh at the Research Improvement Center of Shiraz University of Medical Sciences for improving the use of English in the manuscript.
References
1. In: Edge SB, Byrd DR, Compton CC, Fritz AG, Greene FL, Trotti A. Part II: Digestive system - Colon and rectum. editors. AJCC cancer staging manual. 7th ed. New York: Springer; 2010. p. 143–164.
2. Hoseini S, Moaddabshoar L, Hemati S, Mohammadianpanah M. An overview of clinical and pathological characteristics and survival rate of colorectal cancer in Iran. Ann Colorectal Res 2014;2:e17264.

3. Debunne H, Ceelen W. Mucinous differentiation in colorectal cancer: molecular, histological and clinical aspects. Acta Chir Belg 2013;113:385–390. PMID: 24494463.


4. Hosseini S, Zohourinia S, Zare-Bandamiri M, Mokhtari M, Pourhashemi S, Hosseinzadeh M, et al. Clinical and pathological characteristics of mucinous colorectal adenocarcinoma: a comparative study. Ann Colorectal Res 2016;4:e34404.

5. Kulendran M, Stebbing JF, Marks CG, Rockall TA. Predictive and prognostic factors in colorectal cancer: a personalized approach. Cancers (Basel) 2011;3:1622–1638. PMID: 24212777.



6. Chew MH, Yeo SA, Ng ZP, Lim KH, Koh PK, Ng KH, et al. Critical analysis of mucin and signet ring cell as prognostic factors in an Asian population of 2,764 sporadic colorectal cancers. Int J Colorectal Dis 2010;25:1221–1229. PMID: 20686777.


7. Sung CO, Seo JW, Kim KM, Do IG, Kim SW, Park CK. Clinical significance of signet-ring cells in colorectal mucinous adenocarcinoma. Mod Pathol 2008;21:1533–1541. PMID: 18849918.



8. Thota R, Fang X, Subbiah S. Clinicopathological features and survival outcomes of primary signet ring cell and mucinous adenocarcinoma of colon: retrospective analysis of VACCR database. J Gastrointest Oncol 2014;5:18–24. PMID: 24490039.


9. Safaee A, Moghimi-Dehkordi B, Fatemi SR, Ghiasi S, Nemati-Malek F, Zali MR. . Characteristics of colorectal mucinous adenocarcinoma in Iran. Asian Pac J Cancer Prev 2010;11:1373–1375. PMID: 21198295.

10. Park JS, Huh JW, Park YA, Cho YB, Yun SH, Kim HC, et al. Prognostic comparison between mucinous and nonmucinous adenocarcinoma in colorectal cancer. Medicine (Baltimore) 2015;94:e658PMID: 25881840.



11. Engstrom PF, Arnoletti JP, Benson AB 3rd, Chen YJ, Choti MA, Cooper HS, et al. NCCN Clinical Practice Guidelines in Oncology: colon cancer. J Natl Compr Canc Netw 2009;7:778–831. PMID: 19755046.


12. Nitsche U, Zimmermann A, Späth C, Müller T, Maak M, Schuster T, et al. Mucinous and signet-ring cell colorectal cancers differ from classical adenocarcinomas in tumor biology and prognosis. Ann Surg 2013;258:775–782. PMID: 23989057.



13. Chen JX, Tang XD, Xiang DB, Dong XL, Peng FY, Sun GY. TNM stages and prognostic features of colorectal mucinous adenocarcinomas: a meta analysis. Asian Pac J Cancer Prev 2012;13:3427–3430. PMID: 22994772.



14. Tarantino I, Hüttner FJ, Warschkow R, Schmied BM, Diener MK, Ulrich A. Prognostic relevance of mucinous subtype in a population-based propensity score analysis of 40,083 rectal cancer patients. Ann Surg Oncol 2016;23:1576–1586. PMID: 26714956.



15. Kanemitsu Y, Kato T, Hirai T, Yasui K, Morimoto T, Shimizu Y, et al. Survival after curative resection for mucinous adenocarcinoma of the colorectum. Dis Colon Rectum 2003;46:160–167. PMID: 12576888.


16. Song W, Wu SJ, He YL, Cai SR, Zhang CH, Zhang XH, et al. Clinicopathologic features and survival of patients with colorectal mucinous, signet-ring cell or non-mucinous adenocarcinoma: experience at an institution in southern China. Chin Med J (Engl) 2009;122:1486–1491. PMID: 19719934.

17. Min BS, Kim NK, Ko YT, Baek SH, Lee KY, Sohn SK, et al. Clinicopathological features of signet-ring cell carcinoma of the colon and rectum: a case-matched study. Hepatogastroenterology 2009;56:984–988. PMID: 19760925.

18. Consorti F, Lorenzotti A, Midiri G, Di Paola M. Prognostic significance of mucinous carcinoma of colon and rectum: a prospective case-control study. J Surg Oncol 2000;73:70–74. PMID: 10694641.


19. Purdie CA, Piris J. Histopathological grade, mucinous differentiation and DNA ploidy in relation to prognosis in colorectal carcinoma. Histopathology 2000;36:121–126. PMID: 10672056.


20. Catalano V, Loupakis F, Graziano F, Torresi U, Bisonni R, Mari D, et al. Mucinous histology predicts for poor response rate and overall survival of patients with colorectal cancer and treated with first-line oxaliplatin- and/or irinotecan-based chemotherapy. Br J Cancer 2009;100:881–887. PMID: 19259089.




21. Mohammadianpanah M. Colorectal cancer incidence: does iran follow the West? Ann Colorectal Res 2015;3:e28045.

22. Verhulst J, Ferdinande L, Demetter P, Ceelen W. Mucinous subtype as prognostic factor in colorectal cancer: a systematic review and meta-analysis. J Clin Pathol 2012;65:381–388. PMID: 22259177.


23. Du W, Mah JT, Lee J, Sankila R, Sankaranarayanan R, Chia KS. Incidence and survival of mucinous adenocarcinoma of the colorectum: a population-based study from an Asian country. Dis Colon Rectum 2004;47:78–85. PMID: 14719155.


24. Kang H, O'Connell JB, Maggard MA, Sack J, Ko CY. A 10-year outcomes evaluation of mucinous and signet-ring cell carcinoma of the colon and rectum. Dis Colon Rectum 2005;48:1161–1168. PMID: 15868237.


25. Numata M, Shiozawa M, Watanabe T, Tamagawa H, Yamamoto N, Morinaga S, et al. The clinicopathological features of colorectal mucinous adenocarcinoma and a therapeutic strategy for the disease. World J Surg Oncol 2012;10:109PMID: 22703761.



26. Compton CC, Fielding LP, Burgart LJ, Conley B, Cooper HS, Hamilton SR, et al. Prognostic factors in colorectal cancer. College of American Pathologists Consensus Statement 1999. Arch Pathol Lab Med 2000;12:979–994.
27. Xie L, Villeneuve PJ, Shaw A. Survival of patients diagnosed with either colorectal mucinous or non-mucinous adenocarcinoma: a population-based study in Canada. Int J Oncol 2009;34:1109–1115. PMID: 19287969.


28. Hogan J, Burke JP, Samaha G, Condon E, Waldron D, Faul P, et al. Overall survival is improved in mucinous adenocarcinoma of the colon. Int J Colorectal Dis 2014;29:563–569. PMID: 24425620.


29. Green JB, Timmcke AE, Mitchell WT, Hicks TC, Gathright JB Jr, Ray JE. Mucinous carcinoma: just another colon cancer? Dis Colon Rectum 1993;36:49–54. PMID: 8380140.


30. Shin US, Yu CS, Kim JH, Kim TW, Lim SB, Yoon SN, et al. Mucinous rectal cancer: effectiveness of preoperative chemoradiotherapy and prognosis. Ann Surg Oncol 2011;18:2232–2239. PMID: 21347780.


31. Sengul N, Wexner SD, Woodhouse S, Arrigain S, Xu M, Larach JA, et al. Effects of radiotherapy on different histopathological types of rectal carcinoma. Colorectal Dis 2006;8:283–288. PMID: 16630231.


Fig. 1
Kaplan-Meier survival curves for overall survival categorized according to histologic subtype.
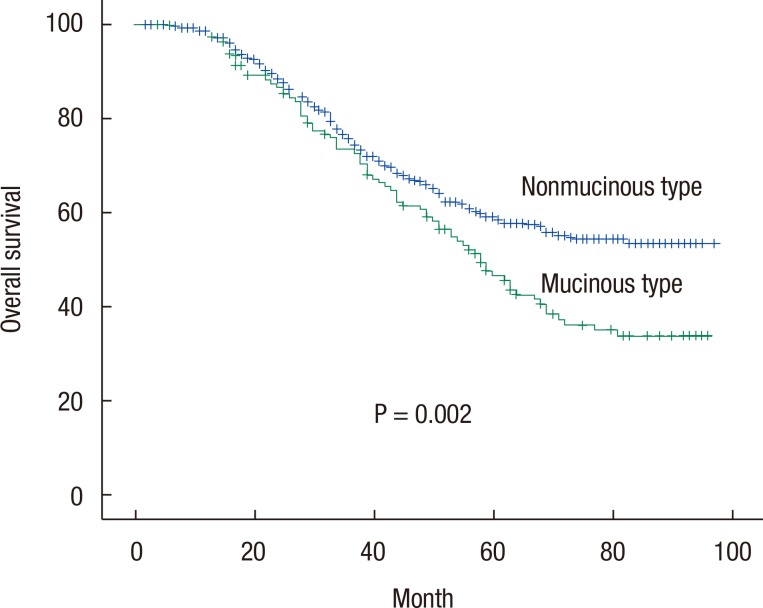
Fig. 2
Kaplan-Meier survival curves for disease-free survival categorized according to histologic subtype.
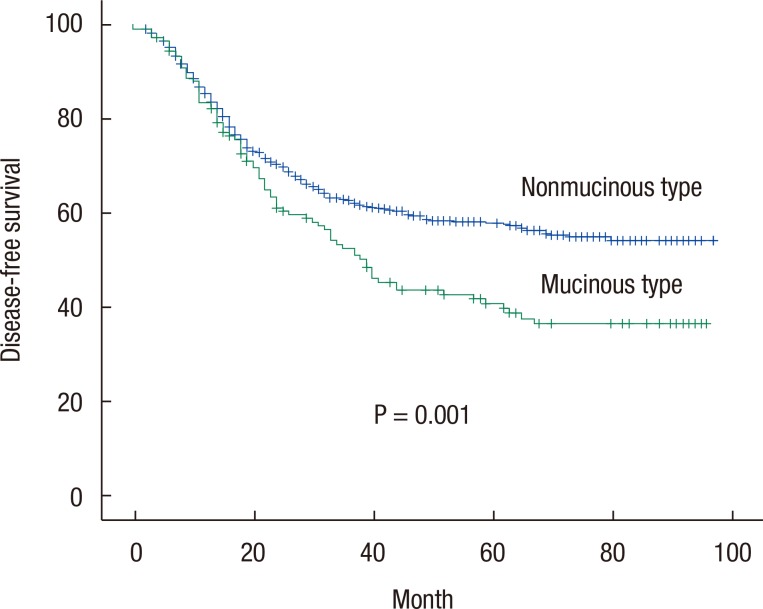
Table 2
Univariate analysis of prognostic factors for disease-free survival in 1,268 patients with colorectal cancer