- Search
Abstract
Purpose
The purpose of this study was to assess the risk factors for repeated abdominal surgery in Crohn's disease (CD) patients after the first abdominal surgery. Prior studies have tried to identify the risk factors for postoperative recurrence in CD patients, but the results of the studies have been inconsistent. Furthermore, few data on the risk factors for repeated abdominal surgery are available.
Methods
Clinical data on CD patients who underwent abdominal surgery from January 2000 to December 2009 were collected from seventeen university hospitals and one colorectal clinic. Data from a total of 708 patients were analyzed to find the risk factors for repeated abdominal surgery in CD patients. The mean follow-up period was 72 months.
Results
The risk of repeated abdominal surgery was 3 times higher in young patients (below 16 years old) than in older patients (odds ratio [OR], 3.056; 95% confidence interval [CI], 1.021 to 9.150); P = 0.046). Stricturing behavior at diagnosis was also a risk factor for repeated abdominal surgery (OR, 2.438; 95% CI, 1.144 to 5.196; P = 0.021). Among operative indications, only intra-abdominal abscess was associated with repeated abdominal surgery (OR, 2.393; 95% CI, 1.098 to 5.216; P = 0.028). Concerning type of operation, an ileostomy might be a risk factor for repeated abdominal surgery (OR, 11.437; 95% CI, 1.451 to 90.124; P = 0.021). Emergency surgery (OR, 4.994; 95% CI, 2.123 to 11.745; P < 0.001) and delayed diagnosis after surgery (OR, 2.339; 95% CI, 1.147 to 4.771; P = 0.019) also increased the risk of repeated abdominal surgery.
Crohn's disease (CD) is heterogeneous in nature; consequently, its clinical course is relatively unpredictable. The only consistent factor in CD is its inconsistency [1]. Some patients have a relatively mild form, but others experience a severe form of CD requiring surgery or have postoperative recurrence. Over 80% of CD patients will undergo surgery, and approximately one-third of those patients will require reoperation [2]. Reported reoperation rates range from 20 to 25% at 5 years after resection and 34 to 39% at 10 years [3, 4]. Several studies have reported the risk factors of an initial intestinal resection or recurrence after the primary operation. Different studies have revealed numerous risk factors for postoperative recurrences, but the results are often not comparable because of differing patient populations and clinical manifestations [5, 6]. In addition, no consistent risk factors for surgery or recurrence, except smoking, have been identified [7, 8]. Furthermore, few studies have evaluated the risk factors for reoperation after the primary surgery in CD patients. Therefore, the aim of the present study was to evaluate the probability of reoperation and to assess the risk factors for reoperation after the primary surgery for CD.
The data for biopsy-proven CD patients who underwent abdominal surgery from January 2000 to December 2009 were collected retrospectively. The operations were performed at 18 different hospitals (17 university hospitals and one colorectal clinic). The factors included in the study protocol were decided at a meeting held before data collection. The data of 754 patients were collected initially, and 46 cases were excluded because of data duplication or unmet criteria (Fig. 1). Data from a total of 708 CD patients were analyzed to determine the risk factors for repeated abdominal surgery. The mean follow-up period was 72 months. The variables that were analyzed were gender, family history, age at diagnosis, disease behavior at diagnosis, and disease location at diagnosis according to the Montreal classification. Other variables were indications, type of first abdominal surgery, and the time interval between diagnosis and surgery.
For the continuous variables, normality was tested first. When the normality assumption was satisfied, a one-way analysis of variance was used; otherwise, a Kruskal-Wallis test was utilized to test whether a mean difference between the number of operations existed (1, 2, Ōēź3). In addition, for the categorical variables, a Pearson chi-square test or a Fisher's exact test was used as appropriate to evaluate the association between the number of operations (1, 2, Ōēź3). In order to evaluate the relationships between the number of operations and the risk factors, we used univariate and multivariate logistic regression modeling. Since the percentage of patients who had more than three operations was only 6.2%, the number of the operations was divided into two categories (1, Ōēź2). Additionally, within the independent variables of surgery type, indication for surgery and main symptoms, a few categories had a low percentage of patients; thus, for the stability of the analysis, those categories were eliminated/merged. For the goodness-of-fit, Hosmer-Leme show statistics were utilized, and the area under the receiver operating characteristic curve was used to assess the model discrimination. All statistical analyses were performed using SPSS ver. 15.0 (SPSS Inc., Chicago, IL, USA).
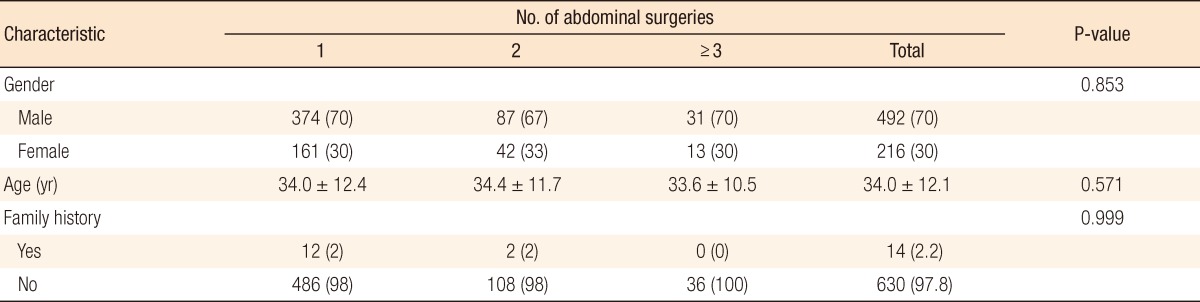
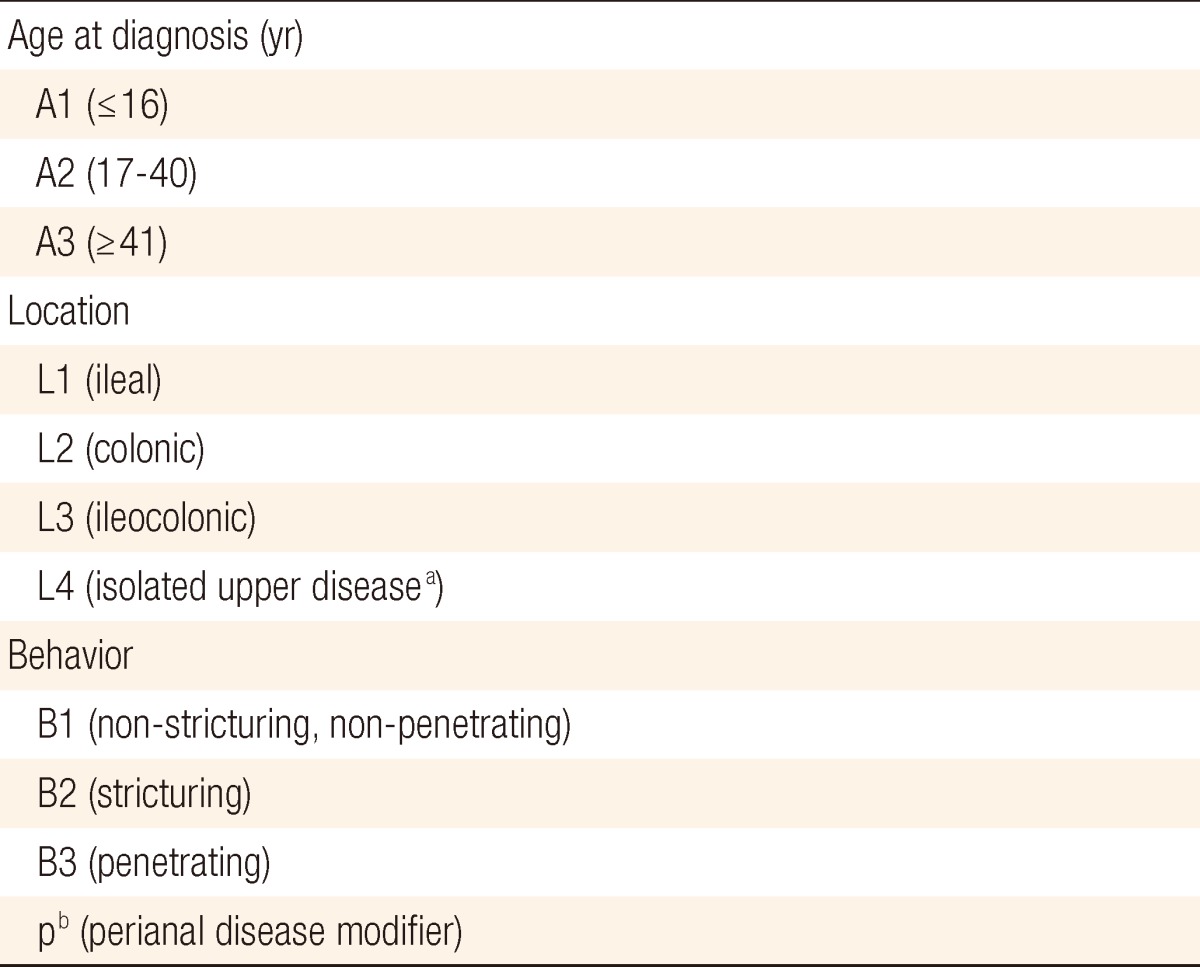
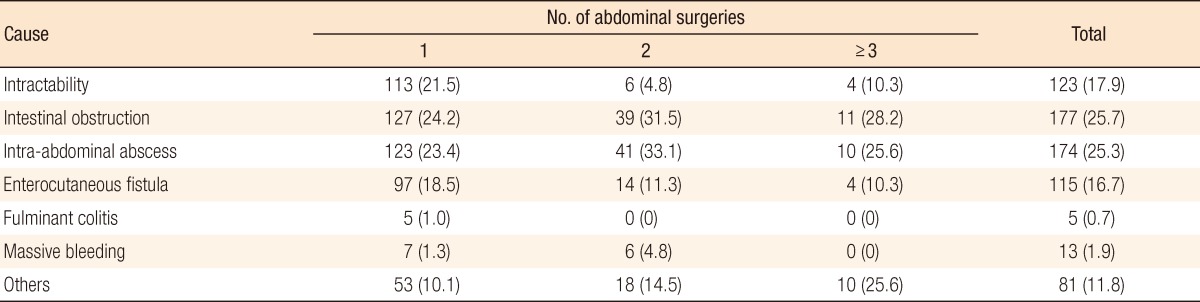
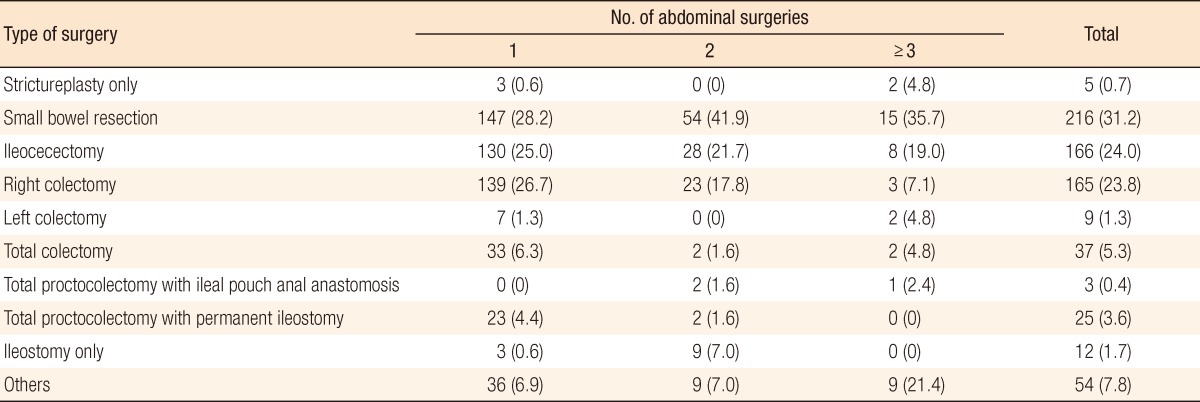
Twenty-four percent of the CD patients with primary abdominal surgery experienced repeated abdominal surgery, and 25% of that 24% underwent one additional abdominal surgery. The male-to-female ratio of the CD patients with abdominal surgery was 2.27:1, and the mean ages of male and female patients were 34.0 and 34.16 years, respectively (Table 1). Family history was confirmed in only 2.2% of the patients. Gender and family history were not associated with repeated abdominal surgery in CD patients. All patients were classified according to the Montreal classification (Table 2). Patients between 17 and 40 years of age (A2), ileal location (L1), and stricturing behavior (B2) were the most common subgroups in the CD patients who underwent primary abdominal surgery (Table 3). Medical intractability (21.5%), intestinal obstruction (24.2%), intra-abdominal abscess (23.4%), and enterocutaneous fistula (18.5%) were common causes of primary abdominal surgery. Intestinal obstruction (31.5%) and intra-abdominal abscess (33.1%) were also common causes of repeated abdominal surgery (Table 4). Small bowel segmental resection (28.2%) was the most common procedure performed in the first abdominal surgery. Of the total number of first abdominal surgeries for CD patients, a right colectomy and an ileocecectomy were performed in 26.7% and 25.0% of the patients, respectively (Table 5).
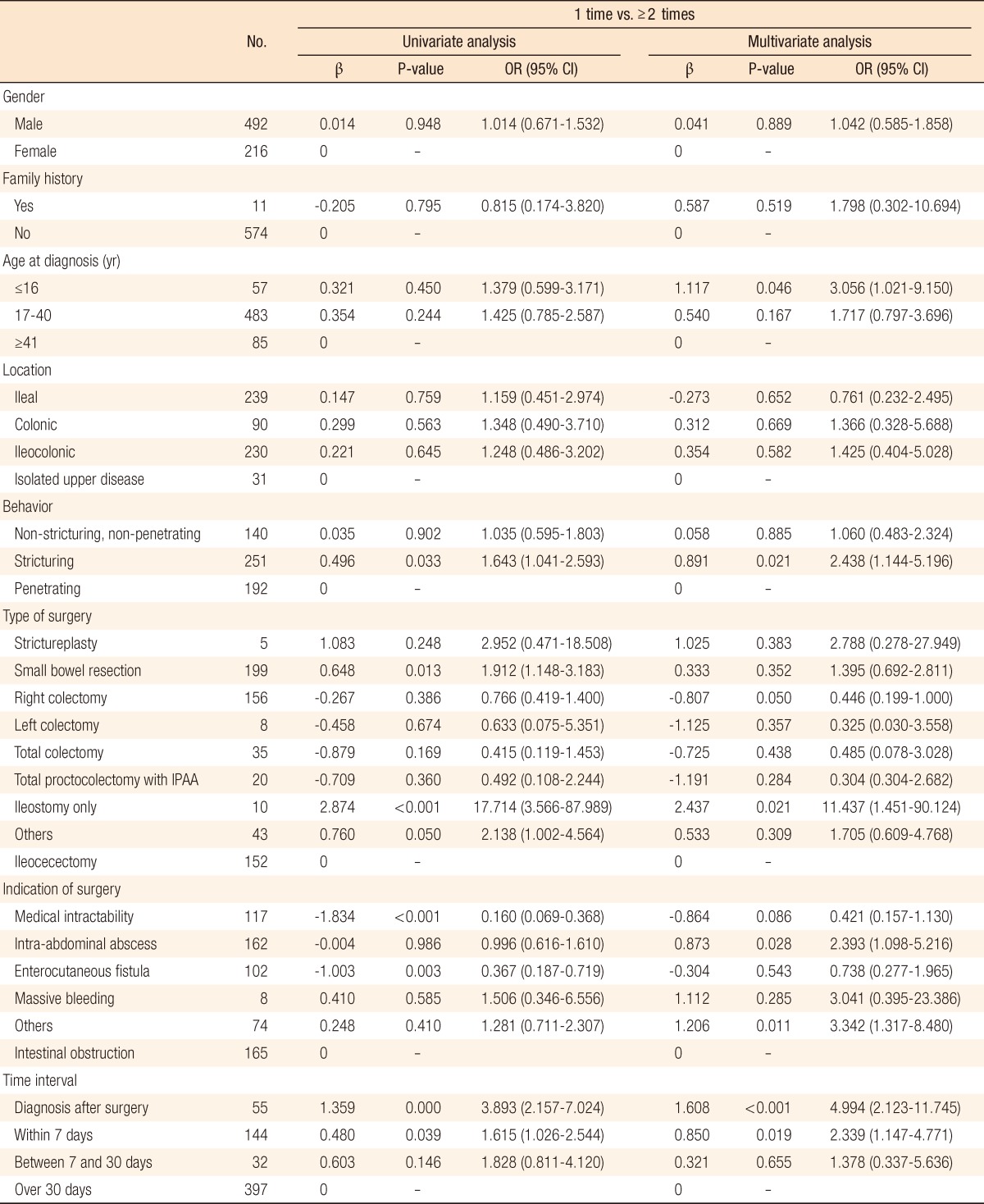
Table 6 summarizes the results of the univariate and the multivariate analyses. The risk of repeated abdominal surgery was approximately three times higher in young patients (under the age of 16 years) than in older patients (odds ratio [OR], 3.056; 95% confidence interval [CI], 1.021 to 9.150; P = 0.046). Stricturing behavior was a greater risk factor for repeated abdominal surgery (OR, 2.438; 95% CI, 1.144 to 5.196; P = 0.021) than was penetrating behavior or non-stricturing and non-penetrating behavior. However, the number of surgeries was not influenced by the location of the disease at diagnosis. Intractability, obstruction, abscess and fistula were the main causes of surgery, and only abscess was associated with repeat surgery (OR, 2.393; 95% CI, 1.098 to 5.216; P = 0.028). Concerning the type of surgery, an ileostomy may be a risk factor for repeat abdominal surgery (OR, 11.437; 95% CI, 1.451 to 90.124; P = 0.021). Emergency surgery (OR, 4.994; 95% CI, 2.123 to 11.745; P < 0.001) and delayed diagnosis after surgery (OR, 2.339; 95% CI, 1.147 to 4.771; P = 0.019) increased the risk for repeat abdominal surgery.
According to the European consensus on definitions and diagnosis of CD, recurrence is primarily used to define the reappearance of lesions after surgical resection while relapse refers to the reappearance of symptoms [9]. Recurrence is the main problem during the treatment of CD. Knowing the risk factors for recurrence would be helpful in managing CD not only for physicians but also for patients. However, due to the heterogeneous nature of CD, the reported risk factors for recurrence after abdominal surgery for CD patients have been inconsistent, so clarifying the risk factors for repeated abdominal surgery in CD patients is difficult. The recurrence rate varies according to the diagnostic method, follow-up duration and ethnicity.
Despite the obvious limitation of using age at diagnosis as a surrogate marker of disease onset, it is nevertheless an attractive, readily available, and stable criterion for distinguishing different disease patterns at diagnosis [10]. With respect to age of onset, the Montreal classification allows for early onset of disease to be categorized separately as a new A1 category for patients with a diagnosis age of 16 years or younger whereas A2 and A3 account for diagnosis ages of 17 to 40 years and of over 40 years, respectively [11]. This change reflects many studies that have reported that specific serotypes or genotypes are more frequently found in early onset CD [12-15]. Early onset CD is usually more severe than A2 or A3 onset. Thia et al. [10] observed that young patients had a tendency toward recurrent clinical flares, indicating a more active disease, and were more likely to receive immunosuppressive therapy than older patients. Polito et al. [16] observed that compared to an older age at diagnosis, defined as individuals older than 40 years of age, a younger age at diagnosis, defined as individuals under 20 years of age, was associated with greater small bowel involvement, more severe stricturing disease, and a higher surgical rate. These results are consistent with the results from the present study. A young age, less than 16 years, was a risk factor for repeated abdominal surgery in CD patients.
Several studies have reviewed early disease onset or diagnosis among CD patients with a family history [16, 17]. Polito et al. [16] postulated that the role of genetic anticipation with greater contribution of maladaptive genes led to an earlier onset of disease manifestation and greater severity in patients with a positive family history. Given that only 2% of the patients in the present study had a positive family history, other reasons may account for young patients experiencing a more severe clinical course than older patients in the present study cohort [10].
Non-stricturing, non-penetrating, stricturing, and penetrating disease behaviors are the main categories in the classification of CD patients. The present study revealed that stricturing disease behavior was associated with repeated abdominal surgery in CD patients. This result is significantly different from other reports. In other studies, penetrating behavior was a risk factor for postsurgical recurrence [8, 18-20]. However, Khoury et al. [21] reported that stricturing behavior was a risk factor for early reoperation. Concerning disease location, several studies demonstrated that the risk of recurrence was highest in ileocolonic CD and lowest in colonic CD [22-24]. In the present study, disease location was not a risk factor for repeat abdominal surgery in CD patients. The influences of disease location and disease behavior on the postoperative recurrence of CD are unclear because these clinical characteristics have been observed to change over time [25].
Among the surgical procedures performed in the first abdominal surgery, only the ileostomy increased the risk for repeated abdominal surgery in CD patients. Because the diseased bowel was not resected in that procedure, an increased reoperation rate was inevitable. However, contrary to other reports, the strictureplasty was not associated with repeated abdominal surgery reports [26-29]. Unlike other reports [30-32], in the present study, the segmental colon resection was not a risk factor for repeated abdominal surgery in CD patients.
Emergency surgery and delayed diagnosis of CD after surgery could increase the risk for repeated abdominal surgery in CD patients. Hellberg et al. [33] demonstrated that no difference in recurrence existed between emergency and elective surgery. A limited resection could not be performed under an emergency situation because determining the extent of resection during emergency surgery was difficult. Understandably, a repeated abdominal surgery could be necessary. Similarly, in the presence of an intra-abdominal abscess, surgeons usually tend to perform fewer surgeries. Therefore, the probability of recurrence might be higher after the first abdominal surgery if the indication for the first operation had been an intra-abdominal abscess.
The present study had several limitations. First, some data were missing because of the retrospective collection technique, which could affect the results. Second, the efficacy of the medical treatment after surgery was not analyzed. Medical treatment, such as the use of immunomodulators or anti-tumor necrosis factor-╬▒, after abdominal surgery for CD could decrease the recurrence rate and affect the results of the present study.
In conclusion, young age (under 16 years of age), stricturing behavior, intra-abdominal abscess, emergency surgery, and delayed diagnosis after surgery may be risk factors for repeated abdominal surgery in Korean patients with CD.
ACKNOWLEDGMENTS
The authors thank members of the Korean IBD study group for considerable help in data acquisition.
References
1. Wolff BG. Factors determining recurrence following surgery for Crohn's disease. World J Surg 1998;22:364ŌĆō369. PMID: 9523518.


2. Heimann TM, Greenstein AJ, Lewis B, Kaufman D, Heimann DM, Aufses AH Jr. Comparison of primary and reoperative surgery in patients with Crohns disease. Ann Surg 1998;227:492ŌĆō495. PMID: 9563535.



3. Goldberg PA, Wright JP, Gerber M, Claassen R. Incidence of surgical resection for Crohn's disease. Dis Colon Rectum 1993;36:736ŌĆō739. PMID: 8348861.


4. Michelassi F, Balestracci T, Chappell R, Block GE. Primary and recurrent Crohn's disease: experience with 1379 patients. Ann Surg 1991;214:230ŌĆō238. PMID: 1929605.



5. Raab Y, Bergstrom R, Ejerblad S, Graf W, Pahlman L. Factors influencing recurrence in Crohn's disease: an analysis of a consecutive series of 353 patients treated with primary surgery. Dis Colon Rectum 1996;39:918ŌĆō925. PMID: 8756849.


6. Anseline PF, Wlodarczyk J, Murugasu R. Presence of granulomas is associated with recurrence after surgery for Crohn's disease: experience of a surgical unit. Br J Surg 1997;84:78ŌĆō82. PMID: 9043461.


7. Cottone M, Rosselli M, Orlando A, Oliva L, Puleo A, Cappello M, et al. Smoking habits and recurrence in Crohn's disease. Gastroenterology 1994;106:643ŌĆō648. PMID: 8119535.


8. Cunningham MF, Docherty NG, Coffey JC, Burke JP, O'Connell PR. Postsurgical recurrence of ileal Crohn's disease: an update on risk factors and intervention points to a central role for impaired host-microflora homeostasis. World J Surg 2010;34:1615ŌĆō1626. PMID: 20195604.


9. Stange EF, Travis SP, Vermeire S, Beglinger C, Kupcinkas L, Geboes K, et al. European evidence based consensus on the diagnosis and management of Crohn's disease: definitions and diagnosis. Gut 2006;55(Suppl 1): i1ŌĆōi15. PMID: 16481628.



10. Thia KT, Luman W, Jin OC. Crohn's disease runs a more aggressive course in young Asian patients. Inflamm Bowel Dis 2006;12:57ŌĆō61. PMID: 16374260.


11. Satsangi J, Silverberg MS, Vermeire S, Colombel JF. The Montreal classification of inflammatory bowel disease: controversies, consensus, and implications. Gut 2006;55:749ŌĆō753. PMID: 16698746.


12. Brant SR, Panhuysen CI, Bailey-Wilson JE, Rohal PM, Lee S, Mann J, et al. Linkage heterogeneity for the IBD1 locus in Crohn's disease pedigrees by disease onset and severity. Gastroenterology 2000;119:1483ŌĆō1490. PMID: 11113069.


13. Rioux JD, Silverberg MS, Daly MJ, Steinhart AH, McLeod RS, Griffiths AM, et al. Genomewide search in Canadian families with inflammatory bowel disease reveals two novel susceptibility loci. Am J Hum Genet 2000;66:1863ŌĆō1870. PMID: 10777714.



14. Russell RK, Drummond HE, Nimmo EE, Anderson N, Smith L, Wilson DC, et al. Genotype-phenotype analysis in childhood-onset Crohn's disease: NOD2/CARD15 variants consistently predict phenotypic characteristics of severe disease. Inflamm Bowel Dis 2005;11:955ŌĆō964. PMID: 16239840.


15. Vasiliauskas EA, Kam LY, Karp LC, Gaiennie J, Yang H, Targan SR, et al. Marker antibody expression stratifies Crohn's disease into immunologically homogeneous subgroups with distinct clinical characteristics. Gut 2000;47:487ŌĆō496. PMID: 10986208.



16. Polito JM 2nd, Childs B, Mellits ED, Tokayer AZ, Harris ML, Bayless TM. Crohn's disease: influence of age at diagnosis on site and clinical type of disease. Gastroenterology 1996;111:580ŌĆō586. PMID: 8780560.


17. Lashner BA, Evans AA, Kirsner JB, Hanauer SB. Prevalence and incidence of inflammatory bowel disease in family members. Gastroenterology 1986;91:1396ŌĆō1400. PMID: 3770366.


18. Simillis C, Yamamoto T, Reese GE, Umegae S, Matsumoto K, Darzi AW, et al. A meta-analysis comparing incidence of recurrence and indication for reoperation after surgery for perforating versus non-perforating Crohn's disease. Am J Gastroenterol 2008;103:196ŌĆō205. PMID: 17900320.


19. Sachar DB, Lemmer E, Ibrahim C, Edden Y, Ullman T, Ciardulo J, et al. Recurrence patterns after first resection for stricturing or penetrating Crohn's disease. Inflamm Bowel Dis 2009;15:1071ŌĆō1075. PMID: 19229992.


20. Mirow L, Hauenschild L, Hildebrand P, Kleemann M, Keller R, Franke C, et al. Recurrence of Crohn's disease after surgery: causes and risks. Zentralbl Chir 2008;133:182ŌĆō187. PMID: 18415909.



21. Khoury W, Strong SA, Fazio VW, Kiran RP. Factors associated with operative recurrence early after resection for Crohn's disease. J Gastrointest Surg 2011;15:1354ŌĆō1360. PMID: 21626229.


22. Farmer RG, Hawk WA, Turnbull RB Jr. Clinical patterns in Crohn's disease: a statistical study of 615 cases. Gastroenterology 1975;68(4 Pt 1): 627ŌĆō635. PMID: 1123132.


23. Farmer RG, Whelan G, Fazio VW. Long-term follow-up of patients with Crohn's disease. Relationship between the clinical pattern and prognosis. Gastroenterology 1985;88:1818ŌĆō1825. PMID: 3922845.


24. Bernell O, Lapidus A, Hellers G. Risk factors for surgery and postoperative recurrence in Crohn's disease. Ann Surg 2000;231:38ŌĆō45. PMID: 10636100.



25. Louis E, Collard A, Oger AF, Degroote E, Aboul Nasr, Belaiche J. Behaviour of Crohn's disease according to the Vienna classification: changing pattern over the course of the disease. Gut 2001;49:777ŌĆō782. PMID: 11709511.



26. Shatari T, Clark MA, Yamamoto T, Menon A, Keh C, Alexander-Williams J, et al. Long strictureplasty is as safe and effective as short strictureplasty in small-bowel Crohn's disease. Colorectal Dis 2004;6:438ŌĆō441. PMID: 15521932.


27. Yamamoto T, Allan RN, Keighley MR. Strategy for surgical management of ileocolonic anastomotic recurrence in Crohn's disease. World J Surg 1999;23:1055ŌĆō1060. PMID: 10512947.


28. Gardiner KR, Kettlewell MG, Mortensen NJ. Intestinal haemorrhage after strictureplasty for Crohn's disease. Int J Colorectal Dis 1996;11:180ŌĆō182. PMID: 8876275.


29. Ozuner G, Fazio VW. Management of gastrointestinal bleeding after strictureplasty for Crohn's disease. Dis Colon Rectum 1995;38:297ŌĆō300. PMID: 7882797.


30. Goligher JC. The long-term results of excisional surgery for primary and recurrent Crohn's disease of the large intestine. Dis Colon Rectum 1985;28:51ŌĆō55. PMID: 3971800.


31. Andrews HA, Lewis P, Allan RN. Prognosis after surgery for colonic Crohn's disease. Br J Surg 1989;76:1184ŌĆō1190. PMID: 2597977.


32. Longo WE, Ballantyne GH, Cahow CE. Treatment of Crohn's colitis: segmental or total colectomy? Arch Surg 1988;123:588ŌĆō590. PMID: 3358685.


33. Hellberg R, Hulten L, Rosengren C, Ahren C. The recurrence rate after primary excisional surgery for Crohn's disease. Acta Chir Scand 1980;146:435ŌĆō443. PMID: 7468077.

- TOOLS
-
METRICS

- Related articles in ACP
-
Risk Factors for Repeat Abdominal Surgery in Patients with Crohn's Disease2012 August;28(4)