- Search
| Ann Coloproctol > Volume 40(2); 2024 > Article |
|
Abstract
Purpose
The estimation of the risk posed by malignant polyps for residual or lymphatic disease plays a central role. This study investigated colorectal surgeonsŌĆÖ assessment of these risks associated with malignant polyps.
Methods
A cross-sectional questionnaire was electronically administered to colorectal surgeons in Australia and New Zealand in October 2022. The questionnaire contained 17 questions on demographics, when surgeons consider colorectal resection appropriate, and the risk assessment for 5 hypothetical malignant polyps.
Results
The mean risk of residual or lymphatic disease that would prompt surgeons to recommend colonic resection was 5%. However, this increased to a mean risk of 10% if the malignant polyp was located in the rectum, and the only resection option was abdominoperineal resection with end-colostomy. There was high concordance between the estimated risk of residual or lymphatic disease by colorectal surgeons and the Association of Coloproctology of Great Britain and Ireland (ACPGBI) guidelines for the 5 hypothetical malignant polyps, with the ACPGBI estimated risk lying within the 95% confidence interval for 4 of the 5 malignant polyps. Nonetheless, 96.6% of surgeons felt that an online risk calculator would improve clinical practice.
Malignant polyps have been defined as any macroscopically complete endoluminal resection of a polyp, containing a focus of adenocarcinoma, invading through the muscularis mucosae, but not beyond the submucosa [1, 2]. After macroscopically complete resection of a malignant polyp, only a small number of patients have residual disease, either within the bowel wall or within the draining lymph nodes [1]. The risk of residual or lymphatic disease is based upon a number of pathological factors, which have been summarised in guidelines, including those developed by the Association of Coloproctology of Great Britain and Ireland (ACPGBI) [3], which prognosticate the risk [4].
It has been previously demonstrated that in an Australian population, a large number of malignant polyps have not been managed per the management recommendations set out in the ACPGBI guidelines. For very-low-risk or low-risk polyps, 31.55% of patients proceeded to colorectal resection, against the recommendations of the guidelines. Additionally, 36.69% of patients with high-risk or very-high-risk polyps underwent polypectomy alone, without proceeding to colorectal resection, which was also against the ACPGBI guidelines [1].
The ACPGBI guidelines were published in 2013 and omit several reporting criteria that would be considered essential in 2022. These include the depth of invasion (as measured in millimetres below the muscularis mucosae) and mismatch repair status [2, 4]. These factors may increasingly play a role in surgeonsŌĆÖ recommendations to patients on treatment options when faced with the diagnosis of a malignant polyp.
This study sought to understand colorectal surgeonsŌĆÖ perception of risk posed by a malignant polyp, and how that risk may be communicated to patients. In Australia and New Zealand, subspecialist colorectal surgeons are represented by the Colorectal Surgical Society of Australia and New Zealand (CSSANZ), which through the Australia and New Zealand Training Board in Colorectal Surgery (ANZTBCRS), facilitates the subspecialist training of colorectal surgeons [5]. This study questioned CSSANZ members (consultant colorectal surgeons) and provisional members (training fellows in colorectal surgery) on the risk perceived by a variety of malignant polyps. We sought to identify how colorectal surgeons in Australia and New Zealand report risks to patients and whether this estimation of risk is concordant with the risks described in a validated set of guidelines published by the ACPGBI.
The study was approved by the St VincentŌĆÖs Private Hospital Northside Human Research and Ethics Committee (No. HREC_22-08_DCLA). All surgeons were provided with a participant information sheet prior to completing the questionnaire, and consent was implied upon completing the questionnaire.
A cross-sectional questionnaire was delivered to all provisional and full practicing members of the CSSANZ in October 2022, with a follow-up reminder sent to nonresponding members and fellows 2 weeks later. All provisional (fellows) and full practicing members (consultants) of the CSSANZ (n=330) were invited via email to participate in the online questionnaire, which was estimated to take between 3 to 4 minutes to complete.
There were 3 components to the questionnaire (see Supplementary Material 1 for the complete questionnaire). Section 1 contained basic demographics, including age, sex, whether the participant was a fellow or a consultant surgeon, time in colorectal surgical practice, and principal practice location. Section 2 assessed the general recommendations the surgeon made upon diagnosis of a malignant polyp, given a healthy patient, without major contraindications to surgery. The final section of the questionnaire assessed the estimation of risk provided to patients, with 5 hypothetical synoptic pathology reports for malignant polyps. The 5 hypothetical malignant polyps are shown in Table 1. The surgeonsŌĆÖ responses to these results were assessed in comparison to the risks attributed in the ACPGBI guidelines for malignant polyps.
The CSSANZ Research Support Committee distributed the questionnaire to the provisional and full practicing members of the CSSANZ by emailing a link to the online REDCap survey [6, 7]. Study data were collected and managed using REDCap electronic data capture tools hosted at the University of Sydney. RED-Cap is a secure, web-based software platform designed to support data capture for research studies [6].
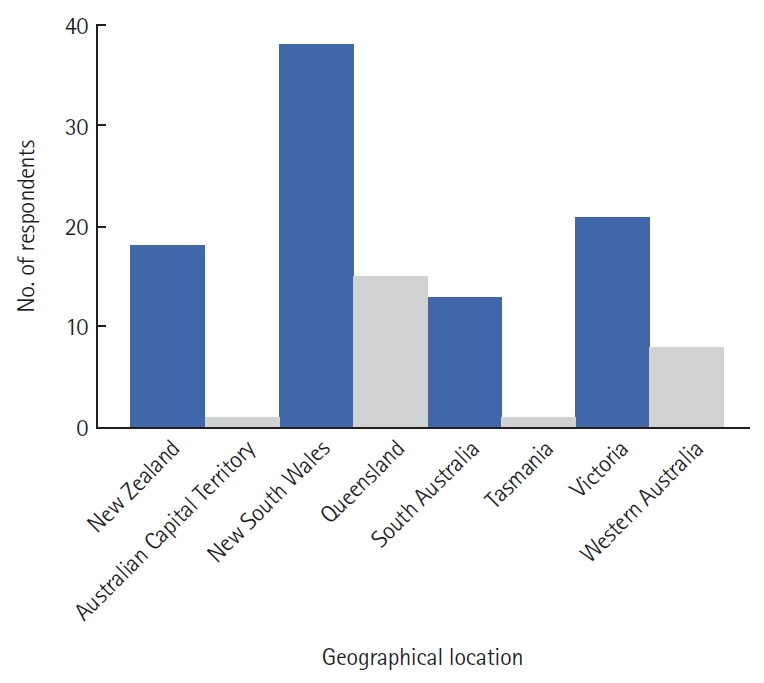
The questionnaire was emailed to 330 members and provisional members of the CSSANZ, with 115 participants (34.8%) responding and 88 participants (76.5%) completing all questions. ParticipantsŌĆÖ demographic characteristics are shown in Table 2. Fig. 1 demonstrates the distribution of questionnaire respondents.
Of those responding, 84 surgeons (73.04%) stated that they discussed all malignant polyps in a multidisciplinary team meeting (MDT) in order for a consensus decision; 30 surgeons (26.3%) reported that they would only discuss selected patients with malignant polyps in an MDT setting. One surgeon never discussed patients with malignant polyps in an MDT.
Surgeons were then surveyed on what risk of residual or lymphatic disease would prompt them to recommend colonic resection for an otherwise healthy patient with a colonic malignant polyp. The median risk for which surgeons were comfortable recommending resection for colonic polyps was 5% (range, 0%ŌĆō20%). The mean risk of residual or lymphatic disease prompting resection did not significantly differ between fellows (mean risk, 7.9%) and consultants (mean risk, 6.2%; P=0.2).
Surgeons were surveyed to see whether there was a difference in recommendation for resection if the malignant polyp was located in the rectum and the only feasible option for rectal resection was abdominoperineal resection (APR) with no option to avoid a permanent end-colostomy. The median risk of residual or lymphatic disease from a malignant polyp that would prompt a surgeon to recommend APR was 10% (range, 0%ŌĆō100%). There was again no statistically significant difference between fellows (mean risk, 23.5%) and consultants (mean risk, 14.6%; P=0.11).
There was a significant difference in the mean risk of residual disease or lymphatic disease between colonic polyps (6.39%) and rectal polyps requiring APR (15.54%) that surgeons felt comfortable recommending resection (P<0.001). Figs. 2 and 3 demonstrate the frequency at which surgeons requested specific investigations after diagnosis for colonic (Fig. 2) and rectal malignant polyps (Fig. 3) to assist in further management recommendations. Other commonly described additional investigations for both colonic and rectal polyps were positron-emission tomography and the blood carcinoembryonic antigen level. Commonly used additional resources to assist in clinical decision-making for malignant polyps were expert pathologists (15.5%) and online risk calculators for early colorectal cancers (9.3%).
Table 1 details 5 hypothetical malignant polyps that surgeons were asked to assess for the risk of residual or lymphatic disease. Table 3 illustrates the mean estimated risk of residual disease or lymphatic disease posed by a variety of malignant polyps in both the colon and rectum, compared to the risk as estimated by the ACPGBI malignant polyp guidelines. There was high concordance between the surgeonsŌĆÖ estimated risk and the ACPGBI estimation of risk, with 4 of the 5 ACPGBI risk calculations lying within the 95% confidence interval of the surgeonsŌĆÖ responses. Lastly, surgeons were questioned whether an online risk calculator would be of use to clinical practice. Of those surgeons surveyed, 96.6% stated that they would use an online risk calculator to help guide the estimation of risk posed by malignant polyps and thus assist in clinical decision-making.
Malignant polyps pose a treatment dilemma for both clinicians and patients. Should patients proceed to colorectal resection, with the associated risks of surgery and also long-term functional changes [8ŌĆō10]? Or can patients be safely managed with polypectomy alone, with some form of regular surveillance? Complicating this decision is the observation that surveillance modalities show poor sensitivity for detecting disease recurrence, especially in draining lymph nodes [11].
Management decisions contrary to the recommendations of the ACPGBI guidelines have been reported. The ACPGBI guidelines state that those polyps rated as either low or very low risk of residual or lymphatic disease should undergo surveillance only. Patients who have malignant polyps with a high or very high risk of residual or lymphatic disease are recommended to proceed to colorectal resection [3] if they are fit enough.
In a population-wide analysis of the management of malignant polyps in Queensland, Australia, 31.55% of very-low-risk or lowrisk polyps proceeded to colorectal resection [1], against ACPGBI guidelines. Amongst the low-risk and very-low-risk group for residual or lymphatic disease, patients who were younger or had right-sided colonic malignant polyps, were more likely to proceed to resection.
Furthermore, 36.69% of patients with high-risk or very-highrisk malignant polyps did not proceed to colorectal resection against the recommendations of the ACPGBI guidelines [1]. Not unexpectedly, those patients who did not proceed to resection amongst this group were more likely to be older, be managed in a public hospital, have left sided colonic polyps, and had retained mismatch repair status on immunohistochemical staining [1].
When surgeons were questioned on what risk of residual or lymphatic disease for which they would recommend an otherwise healthy patient proceed to a colonic resection, the mean response was 5%. However, if the malignant polyp was located in the rectum, and the only possible method of resection was via APR with an end-colostomy, the mean risk at which surgeons would recommend resection doubled to 10%. It is also interesting to note that the converse perception of risk means that surgeons are willing to accept that 90% of patients undergoing APR with end-colostomy would obtain no oncological advantage from the procedure.
This is the first known reported assessment of the perceptions of risk posed by malignant polyps in the literature. Specifically, this study aimed to assess whether surgeonsŌĆÖ estimation of risk of malignant polyps was congruent with the estimation of risk in published guidelines (ACPGBI). Table 3 clearly demonstrates that the mean estimation of risk for the 5 hypothetical malignant polyps was congruent with the estimation of risk from the ACPGBI.
Only polyp 4 had an ACPGBI risk calculation lying outside of the 95% confidence interval of the mean estimation of risk provided by surgeons. There may be several reasons for this. The ACPGBI guidelines would consider polyp 4 a low-risk polyp, with only 1 adverse featureŌłÆa resection margin of 1.5 mm. However, this polyp had several features of borderline significanceŌłÆnamely, moderate differentiation [12], a depth of invasion >1 mm [13] and a 3 mm width of invasion [14]. Whilst these factors do not score adversely on the ACPGBI guidelines, they have been previously reported to increase the risk of residual or lymphatic disease, which might explain why surgeons overestimated the risk of this polyp. Overall, surgeons demonstrated that they were able to accurately assess the risk of malignant polyps relative to each other, with an increasing mean risk of residual or lymphatic disease being estimated for each category of risk defined by the ACPGBI guidelines.
These findings illustrate that the differences between recommended malignant polyp management as per the ACPGBI guidelines and the actual management seen in a population-wide analysis may not be due to surgeonsŌĆÖ inability to estimate the risk posed by malignant polyps; instead, patient preferences may affect the unexpected treatment choices seen in previous analyses.
The ACPGBI guidelines contain several pathological factors for estimating the risk of residual or lymphatic disease: resection margin, Haggitt or Kikuchi level, tumor differentiation, tumor budding, and lymphovascular invasion [3]. However, since the publication of the ACPGBI guidelines in 2013, several pathological factors are now considered to contribute to an increased risk of either residual disease or lymphatic disease, but are not incorporated in these guidelines. In 2004, Ueno et al. [15] reported that width of invasion predicted an increased risk of lymphatic disease from malignant polyps; however, this parameter was not incorporated into the ACPGBI guidelines. The Haggitt and Kikuchi levels are increasingly being replaced with a more standardized direct measure of invasion [16], but this direct measurement of invasion is likewise not included in the ACPGBI guidelines. Additionally, the ACPGBI guidelines do not reflect the updated definitions of budding from the International Tumour Budding Consensus Conference in 2016 [17]. Lastly, whilst mismatch repair status has not been implicated in altering the risk of residual or lymphatic disease, when combined with BRAF testing, mismatch repair status may influence the risk of recurrent disease and thus has implications for management decisions [18, 19]. All of these pathological factors were provided to the surgeons in the hypothetical synoptic malignant polyp reports, and it is interesting to note that they did not significantly change the perception of risk from the described risks from the ACPGBI in 4 of the 5 hypothetical polyps.
The use of online risk calculators for a variety of surgical pathologies has already been demonstrated, including for colorectal cancers [20, 21]. Online risk calculators have the benefit of easy access, and ideally can be accessed using smart devices available in day-to-day clinical practice. Whilst online risk calculators do not replace clinical patient assessment, they can easily help to convey risk to patients and thus assist in the clinical decisionmaking. In the questionnaire, 9.3% of surgeons reported using some form of online risk calculator to assist in the estimation of risk from malignant polyps, such as one for T1 pedunculated polypoid colorectal cancers [22]. However, there currently is no validated online risk calculator for estimating risk for patients diagnosed with malignant polyps. It is, therefore, not surprising to see that 96.6% of surgeons responded that a reliable, online risk calculator for malignant polyps would be of use to their clinical practice. Despite the use of the ACPGBI algorithm in clinical practice, a recent analysis of malignant polyps demonstrated that patients undergoing colorectal resection had improved survival over those who underwent polypectomy alone, even amongst the low-risk and very-low-risk polyp groups [23]. Thus, the future development of guidelines, nomograms, or online calculators for malignant polyps should also incorporate the impacts on survival, and not just residual or lymphatic disease.
There were several limitations to this study. In Australia and New Zealand, colorectal surgery is performed by both colorectal surgeons and general surgeons. This questionnaire was only distributed to subspecialist colorectal surgeons who were members of the CSSANZ. These surgeons may be more cognizant of the pathological factors increasing the risk of residual or lymphatic disease, and may not be truly representative of the overall cohort of surgeons performing colorectal surgery in Australia or New Zealand. Additionally, the questionnaire response rate was 34.8%, and those responding to the questionnaire may also feel more comfortable in their knowledge regarding malignant polyps and be more willing to complete all aspects of the questionnaire. Finally, the responders may not have followed the directions of only consulting the clinical resources they use in daily practice to answer the questions. This issue may have affected the congruency between the questionnaire responses and risk information provided to patients in routine clinical practice.
In conclusion, this is the first published questionnaire on surgeonsŌĆÖ perceptions of risk for patients diagnosed with malignant polyps. Colorectal surgeonsŌĆÖ estimation of risk for a variety of malignant polyps was largely congruent with that of the published ACPGBI guidelines. Despite this congruency between guidelines and the individual surgeonsŌĆÖ assessment of risk, 96.6% of surgeons felt that an online risk calculator would facilitate improved patient care.
Notes
Supplementary materials
Supplementary Material 1.
Questionnaire provided to colorectal surgeons.
Supplementary materials are available from https://doi.org/10.3393/ac.2023.00178.0025.
Fig.┬Ā2.
Investigations ordered for colonic malignant polyps. CT, computed tomography; CAP, chest abdomen and pelvis; CXR, chest x-ray; MRI, magnetic resonance imaging; US, ultrasound.

Fig.┬Ā3.
Investigations ordered for rectal malignant polyps. CT, computed tomography; CAP, chest abdomen and pelvis; CXR, chest x-ray; MRI, magnetic resonance imaging; US, ultrasound.

Table┬Ā1.
Five hypothetical malignant polyps used in the study questionnaire
Table┬Ā2.
Demographics of responding surgeons
Table┬Ā3.
Estimated risk of residual or lymphatic disease compared to the risk estimated from ACPGBI guidelines
REFERENCES
1. Zammit AP, Panahi SE, Brown I, Hooper JD, Clark DA, Riddell AD. Management of high and low risk malignant polyps: a population-wide analysis. Colorectal Dis 2023;25:66ŌĆō74.




2. Zammit AP, Lyons NJ, Chatfield MD, Hooper JD, Brown I, Clark DA, et al. Patient and pathological predictors of management strategy for malignant polyps following polypectomy: a systematic review and meta-analysis. Int J Colorectal Dis 2022;37:1035ŌĆō47.




3. Williams JG, Pullan RD, Hill J, Horgan PG, Salmo E, Buchanan GN, et al. Management of the malignant colorectal polyp: ACPGBI position statement. Colorectal Dis 2013;15 Suppl 2:1ŌĆō38.


4. Zammit AP, Brown I, Hooper JD, Clark DA, Riddell AD. Missing parameters in malignant polyp histology reports: can appropriate decisions be made? Pathology 2023;55:58ŌĆō63.


5. Colorectal Surgical Society of Australia and New Zealand (CSSANZ). About [Internet]. CSSANZ; c2013 [cited 2022 Dec 26]. Available from: https://cssanz.org/training
6. Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG. Research electronic data capture (REDCap): a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform 2009;42:377ŌĆō81.



7. Harris PA, Taylor R, Minor BL, Elliott V, Fernandez M, OŌĆÖNeal L, et al. The REDCap consortium: building an international community of software platform partners. J Biomed Inform 2019;95:103208.



8. Kirchhoff P, Clavien PA, Hahnloser D. Complications in colorectal surgery: risk factors and preventive strategies. Patient Saf Surg 2010;4:5.




9. Giglia MD, Stein SL. Overlooked long-term complications of colorectal surgery. Clin Colon Rectal Surg 2019;32:204ŌĆō11.



10. McGiffin T, Clark DA, Edmundson A, Steffens D, Stevenson A, Solomon M. Surgical management and long-term functional outcomes after anastomotic leak in patients undergoing minimally invasive restorative rectal resection and without a diverting ileostomy. ANZ J Surg 2022;92:806ŌĆō12.



11. Zammit AP, Brown I, Hooper JD, Clark DA, Riddell AD. Timing of surveillance colonoscopy following malignant colorectal polypectomy in Queensland. ANZ J Surg 2023;93:606ŌĆō11.



12. Xu W, He Y, Wang Y, Li X, Young J, Ioannidis JP, et al. Risk factors and risk prediction models for colorectal cancer metastasis and recurrence: an umbrella review of systematic reviews and meta-analyses of observational studies. BMC Med 2020;18:172.




13. Hagen CE, Farooq A. Histologic evaluation of malignant polyps and low-stage colorectal carcinoma. Arch Pathol Lab Med 2019;143:1450ŌĆō4.



14. Brown IS, Bettington ML, Bettington A, Miller G, Rosty C. Adverse histological features in malignant colorectal polyps: a contemporary series of 239 cases. J Clin Pathol 2016;69:292ŌĆō9.


15. Ueno H, Mochizuki H, Hashiguchi Y, Shimazaki H, Aida S, Hase K, et al. Risk factors for an adverse outcome in early invasive colorectal carcinoma. Gastroenterology 2004;127:385ŌĆō94.


16. Royal College of Pathologists of Australasia (RCPA). Polypectomy and local resections of the colorectum structured reporting protocol. 2nd ed. RCPA; 2020.

17. Lugli A, Kirsch R, Ajioka Y, Bosman F, Cathomas G, Dawson H, et al. Recommendations for reporting tumor budding in colorectal cancer based on the International Tumor Budding Consensus Conference (ITBCC) 2016. Mod Pathol 2017;30:1299ŌĆō311.



18. Rodriguez-Bigas MA, Boland CR, Hamilton SR, Henson DE, Jass JR, Khan PM, et al. A National Cancer Institute Workshop on Hereditary Nonpolyposis Colorectal Cancer Syndrome: meeting highlights and Bethesda guidelines. J Natl Cancer Inst 1997;89:1758ŌĆō62.


20. Lo SN, Ma J, Scolyer RA, Haydu LE, Stretch JR, Saw RP, et al. Improved risk prediction calculator for sentinel node positivity in patients with melanoma: the Melanoma Institute Australia nomogram. J Clin Oncol 2020;38:2719ŌĆō27.



21. Mahjoub M, Sioson L, Sheen A, Ahadi M, Chou A, Gill AJ, et al. Predicting survival in colorectal carcinoma after curative resection: a new prognostic nomogram. Pathology 2022;54:79ŌĆō86.


- TOOLS
-
METRICS

-
- 0 Crossref
- Scopus
- 1,165 View
- 93 Download
- Related articles in ACP
-
The Benefits of Colorectal Surgery Surveys in Australia and New Zealand 2020 April;36(2)